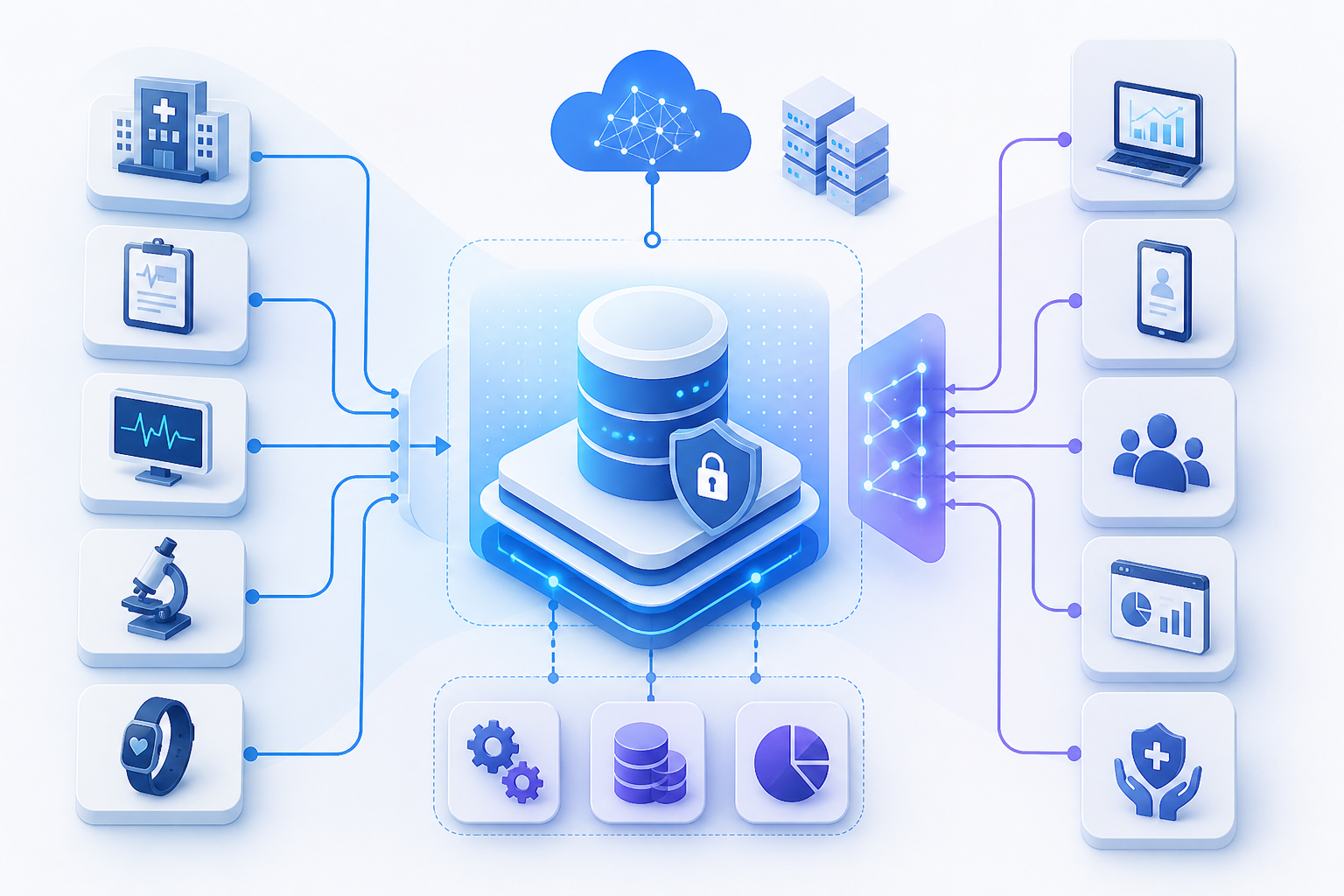
When you integrate multiple healthcare systems, the accuracy of healthcare data makes the difference between safe care and silent risk. Every feed, every interface, and every mapping choice either protects or erodes clinical decisions.
You already know integration is not optional. Health systems run on EMRs, practice management platforms, revenue cycle tools, HIEs, and an expanding stack of eCommerce-like patient engagement solutions. What you control is how reliable your shared data becomes as it moves between them.
In this guide, you will see where the accuracy breaks, how to design validation into your data flows, and how strong healthcare data governance holds it together at scale. It keeps the focus on the practical so that one can apply it across his or her own multi-system integration footprint.
Causes of Inaccuracy
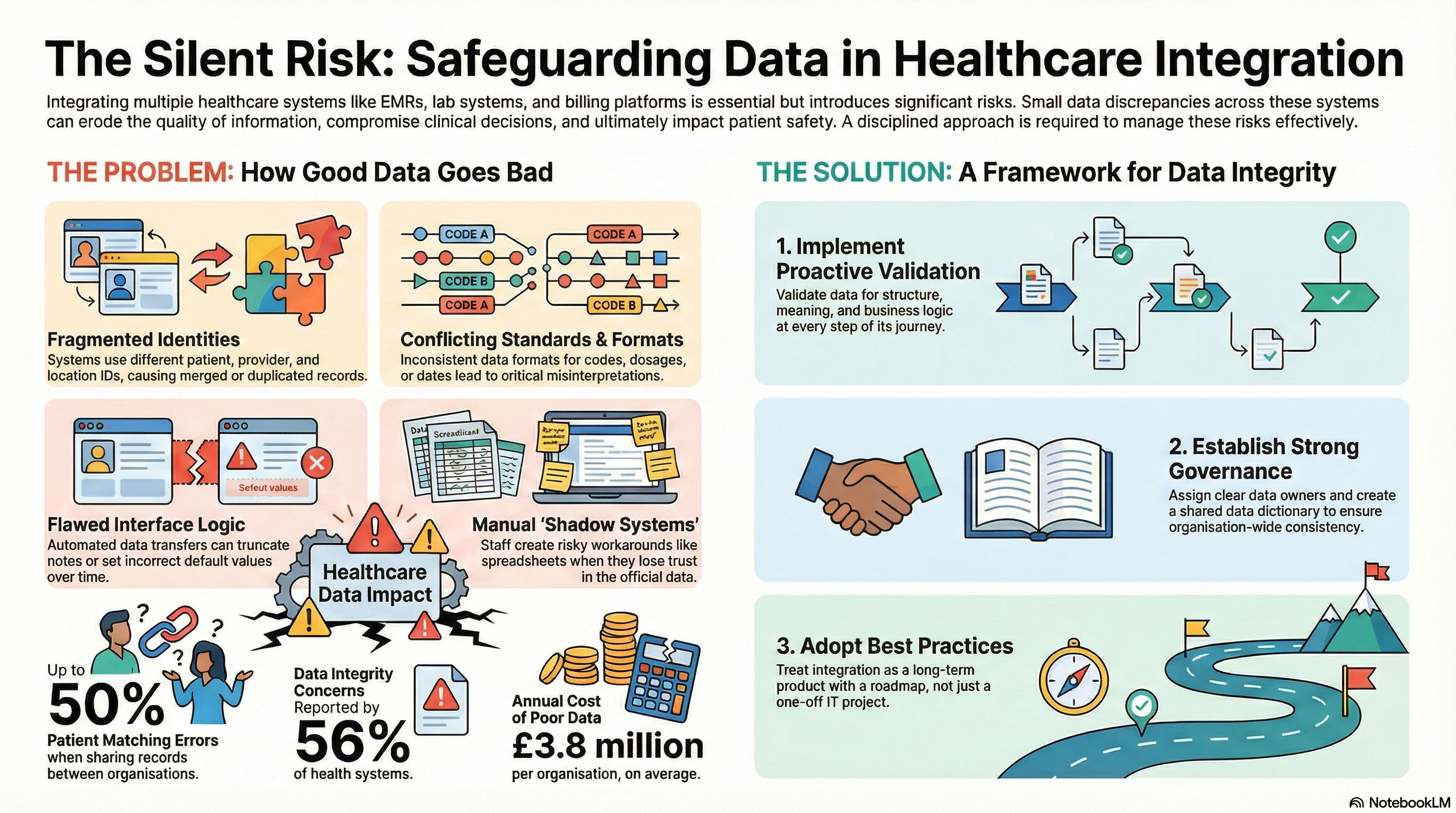
You have to understand the source of the problem before you can mend the accuracy of the healthcare information. In multi-system integration, there isn’t going to be one disastrous event causing the trouble. It will all begin with tiny discrepancies.
1. Inconsistent identifiers across systems
The most pervasive root cause has to be identity. Patients, providers, locations, and payers never have a globally shared truth in your integrated systems. Your EMR system uses a medical record number, your other EMR system uses an enterprise ID, your lab system maintains a patient key, and your CRM system maintains a different ID.
Without a uniform master identifier approach, you risk:
- Replicated Patient Records in Receiving Systems
- Merged charts that involve the wrong people
- Multiple records of clinical history
According to the Journal of AHIMA, patient matching error rates ranged from 8 percent to 12 percent within an institution and up to 50 percent when records are retrieved from other sources.
2. Variations in data standards and formats
Even if you have shared identifiers, the quality of healthcare data is compromised if systems use different dialects of a given standard. This occurs each day with:
- HL7 v2 messages with site-specific Z segments
- Incompatible extension of FHIR resources
- Local codes combined with LOINC, SNOMED CT, or RxNorm.
- Date, time, and unit values with inconsistent formats
Such differences cause errors. For instance, a drug dosage reported in milligrams but recorded in grams, or a regional lab code assigned an inappropriate LOINC code. In JAMIA Literature Review, it was reported that the mismatch in the assignment of laboratory codes results in the reclassification of test result data in up to 15 percent of patient cases when reusing data.
3. Interface logic that mutates meaning
Multi-system integration logic is another source of drift. Each interface engine, ETL job, or API transformation layer applies its own set of rules. Dozens of mappings and conditionals change the shape and context of your data over time.
Common examples include
- Truncation of lengthy text fields such as clinical notes
- Conditional mappings to set default values on empty fields
- Normalization logic that discards all unusual codes or values
- One-way flows, which never send corrections or late updates
None of them is extreme on its own. Combined, they contribute to degradation in the coherence of EMR data and, by implication, to making audit trails harder to reconstruct.
4. Manual workarounds and local shadow systems
When your care team and staff lack trust in integrated data, they will use spreadsheets, homegrown databases, and manual processes to close the gap. The result is a “shadow IT system,” which can circumvent the typical data integration routes and exist outside the governing structure.
The result of:
- Inconsistent patient rosters and panel definitions
- Variants of information on drugs and allergies according to the department
- Gaps between operational reports & EMR
A concern for data integrity has been found in 56 percent of health systems analyzed by KLAS research, due in part to the lack of integration logic.
Validation Techniques
After understanding why, you have to learn methods to safeguard data integrity in healthcare. Validation must be at one point alone. It has to be visible at Ingest, Transformation, and Consumption.
1. Schema validation at every interface boundary
Begin validation for all schemas for both incoming and outgoing feeds. Additionally, for the HL7, FHIR, CSV, and flat file interfaces, enforce the structure before transforming.
Practical actions:
- Establish message profiles for HL7 and reject all unformatted messages
- Use validation profiles defined by FHIR for resources received from partners
- Execute schema checks for required columns, data types, and value ranges for the inputted CSV data
- Failure logging and routing for supporting error handling in queues
This safeguards you against malformed data even before it goes into clinical operations and financial operations, thus preventing costly rework within your data validation processes for healthcare.
2. Referential and cross-system checks
“Format” is protected from data errors in a Schema Validation operation. “Meaning” is safeguarded in a Referential Validation process. It is necessary to have tests that ensure that a reference to a known person, a known provider, a known site, a known order, and that all associated values match.
Techniques to apply:
- Verify that patient identifiers exist in your master person index
- Match provider and location identifiers to formal reference tables
- Validate relationships like orders and results against the source system
- Identification of orphaned records, for example, laboratory results without any associated order or patient
The Office of the National Coordinator revealed that a challenge in the matching of patients when data is shared with other organizations affected 40 percent of the country’s hospitals, thus inhibiting the integration process because referential integrity is paramount.
3. Business rule validation for clinical and operational logic
Even after successfully passing structural and referential checks, business rules need to be validated. Business rules represent how your business considers data to be valid and meaningful.
Examples:
- Age groups for pediatric or geriatric care based on visit type
- Unmatched combinations of diagnoses and procedural codes
- Interaction between medication routes and ordered medications
- Units of measure corresponding to a given lab or vital
These essentially have to be integrated into either your integration platform or validation layer. When it comes to healthcare data validation workflow, you should begin with a small number of high-impact rules and gradually build from there.
4. Statistical and anomaly detection
Some data quality issues do not manifest themselves in the form of simple rule violations. They show up as shifts in distributions, unexpected changes in volumes, or anomalies in patterns. For multi-system integration, anomaly detection helps you surface integration issues before end users report them.
Useful techniques:
- Monitor message or API call volumes by source and type
- Track distributions of key values, such as encounter counts by location
- Alerting on a sudden drop or spike in certain message types or code sets
- Employing simple statistical thresholds before complex machine learning models
A report by the Ponemon Institute estimated the average cost of poor data quality in healthcare at $4.9 million per year per organization, driven in part by undetected anomalies that affect revenue cycle and clinical performance metrics.
Governance
Validation gives you control at the technical level. Healthcare data governance gives you control at the organizational level. Without governance, every project team defines its own rules, code mappings, and quality thresholds, which pulls healthcare data accuracy in different directions.
1. Define clear data ownership
You require individuals or entities as owners for the major data domains. Data ownership cannot remain the province of information technology alone. The domain owners include clinicians and individuals with ownership in the operation and cost aspects of data.
A practical model:
- Owner of clinical data regarding diagnosis, procedures, orders, results, and documentation
- Data Owner: patient demographics, identifier, and consent
- Provider and staff data owner regarding clinician identities and roles
- Financial information owner regarding charges, payments, and payer enrollment information
These owners review code sets, data definitions, and integration requirements, as well as help with triage when accuracy issues are discovered.
2. Shared definitions and data cataloging
Governance must also provide a common vocabulary. Even if your pipelines run flawlessly, if different teams assign different meanings to the same term, there goes the consistency in your EMR data.
Critical actions:
- Business glossary: maintain agreed definitions for core metrics and entities
- Document how each metric is calculated, and from which systems
- Map physical fields in the EMRs, billing, and ancillary systems to shared definitions
- Publish this information via a searchable data catalog
According to Gartner, organizations lose an average of 12.9 million dollars annually due to poor data quality alone, with reconciliation required because of conflicting definitions and reports being one of the major contributors to this statistic.
Healthcare data governance cuts waste by aligning definitions across multi-system integration work.
3. Governance for code sets and standards
Coding standards sit at the center of healthcare data accuracy. Your governance model should indicate what standards apply to what domains and how you manage local extensions.
You should:
- Adopt standard vocabularies, including ICD-10-CM, CPT, LOINC, SNOMED CT, and RxNorm
- Define processes to add or retire local codes and map them to standards
- Control who can create new codes in each source system
- Maintain central mapping tables for cross-system translations
This allows consistent interpretation across EMRs, analytics platforms, and external partners regarding diagnoses, procedures, labs, and medications.
4. Governance workflows for issue management
Even with your strongest designs, data quality issues will manifest. Governance provides a way for your team to react to and remediate such issues.
Construct workflows to:
- Enable end-users to easily point out problems with the data that relate to certain patients or records
- Route issues to owners of relevant domains and integration teams
- Monitor root causes rather than just corrective measures
- Use Learnings to improve validation rules and training
A more visible and trustworthy aspect of healthcare data governance is when care providers notice the timely resolution of issues, not just for one system, but for the root cause itself.
Best Practices
With validation methodologies and foundations of governance in place, you are ready to establish specific practices to support healthcare data integrity in multi-system integration initiatives.
1. Treat integration as a product, not a project
Integration projects invariably begin with the implementation of a new EMR, CRM solution, or patient access system. And then comes the endless stream of interfaces. They all need to be maintained, updated, and improved.
Your integration platform should be treated as a product in the following ways:
- Product stewardship and roadmaps
- Backlog of improvements in data quality and accuracy
- Service level goals for availability and latency of the data
- Clinical and operational reviews
This paradigm shift integrates the work of data integration into long-term healthcare data accuracy rather than one-time delivery.
2. Standardize patterns for common integrations
In many cases, there are similar patterns in the different integrations. To avoid risks associated with different patterns in the various integrations and to improve the quality and speed of
- Patient registration interfaces for EMR, CRM, and billing
- Order and outcome workflow between labs, radiology, and EMRs
- Scheduling the data into patient access and reminder tools
- Clinical documentation & summarization for use in analytics platforms
For each pattern, establish the definition for the reference mappings, validation, monitoring, and common code sets to ensure consistency with the EMR data across new projects and to streamline designs.
3. Build test data and regression suites
To protect your live data, you have to invest in test data and regression tests. The integration effort between multiple systems tends to regress because vendors tend to update, you introduce a new field, and new facilities come into place.
Effective practice includes:
Being open
- Review test data that includes edge cases, for example, variations of last name, difficult orders, and unusual encounters.
- Automatic interface tests for the schema as well as key business rules before every deployment
- Versioning system for mappings and transformations with a clean history of changes
- Provide release checklists involving detailed steps for healthcare data validation
If you view integration change as software change, your accuracy levels remain constant during upgrades as well as new integrations.
4. Close the feedback loop with end users
Those who are impacted by bad information are your clinicians, your revenue cycle staff, and your operational leaders. You should invite this perspective in.
While there is no definitive list
- Regular meetings with the key service line clinical champions
- Easy methods for marking questionable database records from the clinical systems
- Common dashboards for viewing data quality trend charts and incident numbers
- Transparency relating to root causes and actions taken
This not only increases the strength of trust in integrated data, but it also keeps your own priorities straight and aligned with real-world risks, as opposed to purely technological ones.
5. Align integration with security and privacy
The accuracy of healthcare data is not distinct from the concepts of security and privacy. It is affected by identity management, access, consent, the data that flows, and the accuracy of every view.
Best Practices:
- Implement identity and access management for shared PHI systems centrally
- Consent sharing and consent requirements should be incorporated into the design of the integration, not treated as an add-on or an afterthought.
- Track who views the combined views and how they utilize the exported datasets
- Coordinate incident response plans across integration, security, and privacy groups
When integration, governance, and security come together, multi-system integration enables safe data use for care, operations, research, and eCommerce-type engagement.
Conclusion
Accuracy in multi-system integrated healthcare data is not a project deliverable; it’s a discipline. Every identifier, mapping, transformation, and governance decision either supports or erodes the quality of the information that clinicians depend upon.
You are truly setting up your organization for safer care, better analytics, and more reliable digital experiences by embedding the root causes of inaccuracy at every stage and building strong healthcare data governance.
You don’t have to tackle everything at once. Start with one integration path, one data domain, and a single set of validation rules. Then measure your gains, expand your patterns, and share your wins. Over time, these steps compound into a durable integration fabric that your clinicians trust and your executives rely on.
FAQs
What is the accuracy of healthcare data about integration?
Accuracy in health care data integration means that data moving across systems represents the real clinical or operational situation without distortion. This includes the right values, right context, right patient or provider, and right timing so that downstream systems can act on it safely.
How does multi-system integration bear on patient safety?
Multisystem integration impacts patient safety when inaccurate or incomplete data reaches clinical decision points, leading to wrong allergies, outdated medication lists, or missing results that may precipitate unsafe orders or delayed treatment. Precise integration enables complete, current views of the patient throughout the care continuum.
Which data validation in healthcare do I have to apply first?
Start with schema validation and referential checks. These two steps will catch the largest share of structural errors and identity issues with manageable effort. Then add high-impact business rules for medications, allergies, and orders before going on to more advanced anomaly detection.
How can I ensure that the data on EMR is consistent from one facility to another?
It’s also important to establish standard code sets, templates, and workflows for EMR data consistency across facilities. The master person index should be shared with the common provider and location reference tables. Integration patterns for registration, orders, and results need to be aligned and enforced through governance and testing.
What role does healthcare data governance play in analytics initiatives?
Analytics initiatives rely on consistent, accurate data across numerous sources. Healthcare data governance sets the definitions, ownership, and quality expectations that keep analytics stable. Without governance, analysts spend most of their time reconciling definitions in conflict and fixing upstream issues instead of generating insights.
How Vorro Helps You Strengthen Healthcare Data Accuracy?
Vorro is all about integrating healthcare to maintain ‘Data accurate, consistent, and ready for action clinically’. The Vorro platform and team come together to provide consistency in the interfaces you design, define validation rules, and enforce consistent mappings across your EMRs, revenue cycle tools, and digital engagement solutions.
If one needs to simplify multi-system integration while improving healthcare data accuracy, then Vorro can help create an integration strategy that clinicians and leaders alike will have confidence in.
Akshita is a Senior Content Writer and Marketer with over a decade of experience crafting narratives that convert, rank, and build lasting brand authority. She has worked across SaaS, FinTech, HealthTech, and Education spaces, delivering everything from HIPAA-compliant medical content to multilingual campaigns for the International Labour Organization, United Nations. Her content has reached audiences across the globe, and she has worked for Fortune 500 brands, global agencies, and startups alike. Fluent in English, Spanish, and German, Akshita brings a rare cross-cultural edge to brand communication. A literature graduate from Delhi University, she balances strategic thinking with a storyteller's instinct, but when she isn’t architecting content roadmaps, she channels her creativity into poetry and painting or dedicates her time to caring for stray animals - pursuits she credits for making her a more empathetic and perceptive communicator.