You feel the pressure from every side. Clinical teams want simpler workflows. Patients expect digital convenience. Leaders push for innovation that produces real outcomes. Yet your systems hold data in silos, your teams copy and paste information, and every new solution seems to add complexity instead of clarity.
This is where the importance of healthcare interoperability becomes clear to you. Interoperability is no longer a technical project. It is the foundation for healthcare innovation technology, sustainable operations, and connected care models that support your strategy.
If you lead digital, clinical, or operational transformation, you need a practical view of how interoperable healthcare systems support innovation, what holds you back, and how to move from fragmented data to a connected healthcare ecosystem that performs at scale.
What Is Healthcare Interoperability
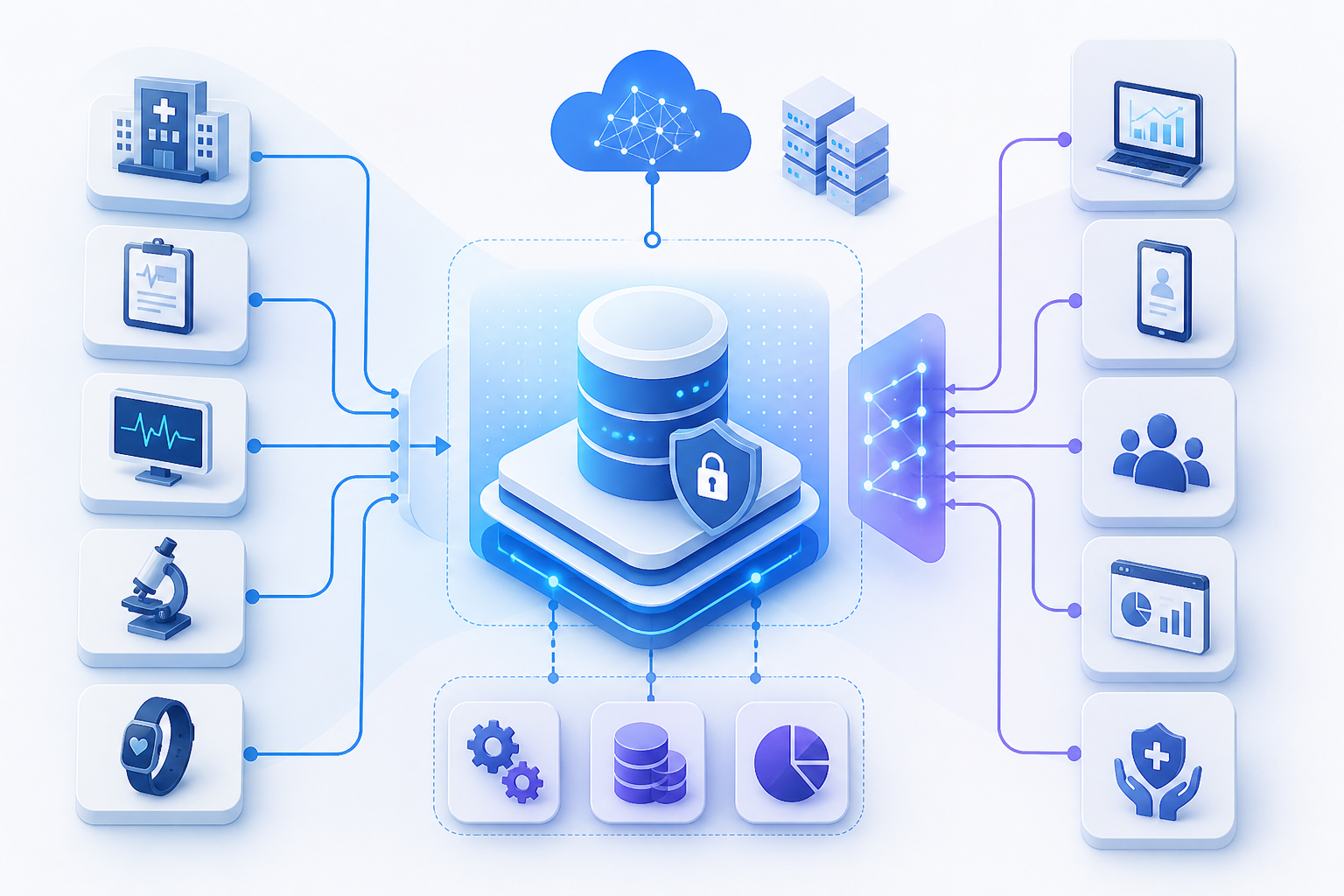
Healthcare interoperability is the ability of different systems, applications, and devices to exchange, understand, and use health data consistently. It is not only about moving data from one place to another. The data must keep its meaning and context so that every system and user can rely on it.
When you focus on healthcare data interoperability, you look at three outcomes:
- Data moves securely between systems.
- Data keeps the same meaning everywhere.
- Data supports decisions, workflows, and reporting without manual rework.
The importance of healthcare interoperability becomes clear when your EHR, lab system, pharmacy, imaging, population health tools, and digital front door solutions all speak a shared language, even if they come from different vendors.
Types of Healthcare Interoperability
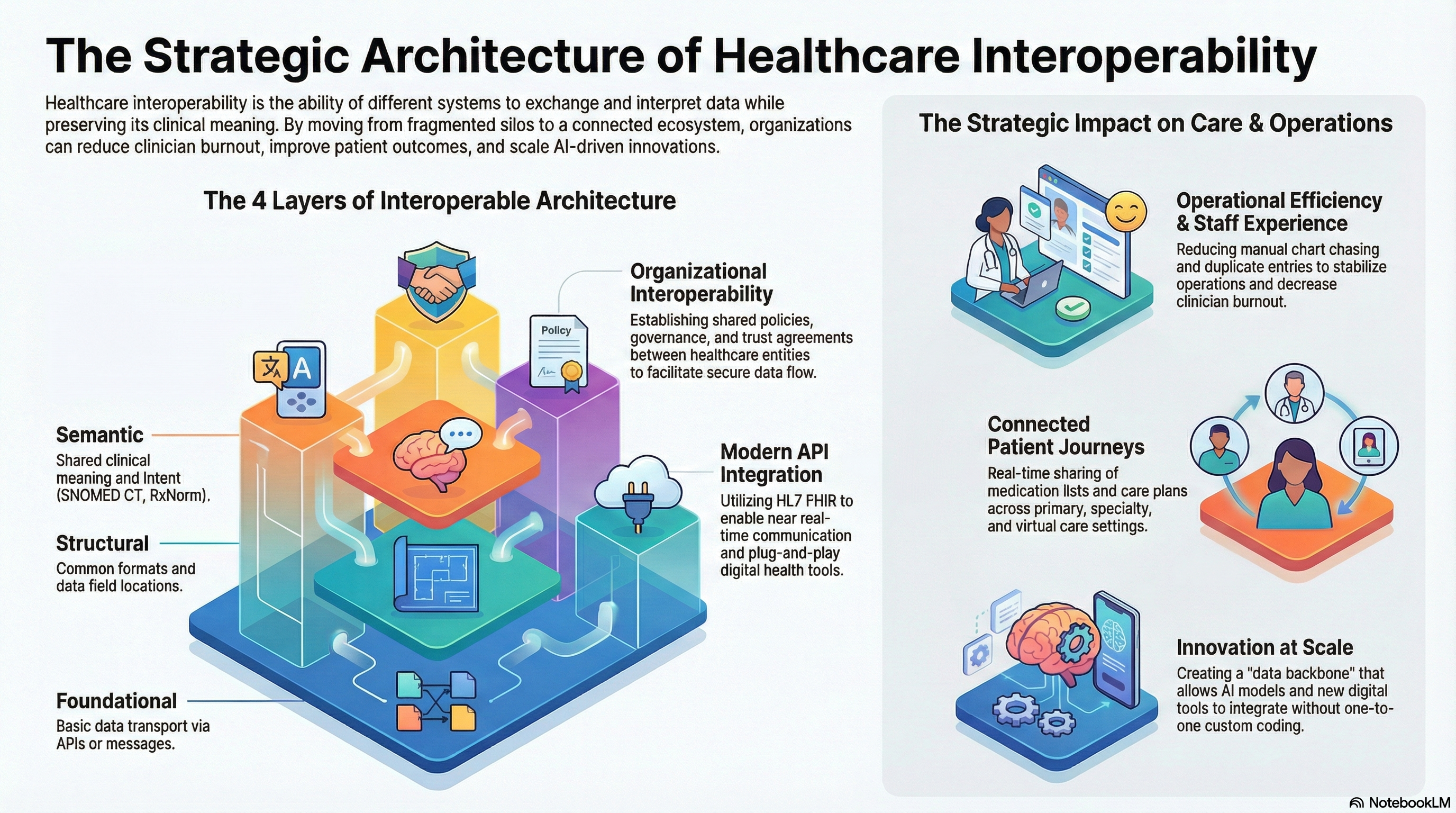
To design interoperable healthcare systems, you need clarity on the layers of interoperability. Each layer solves a different part of the problem.
Foundational interoperability
This level focuses on basic data exchange. Systems send and receive information, for example, through HL7 messages or APIs. At this level, a system can transport data but may not fully interpret it without additional mapping.
Structural interoperability
Here, healthcare data interoperability includes a shared structure. Both the sender and the receiver use a common format for fields and segments. This is where standards such as HL7 and CDA models play a role, ensuring data is stored in known locations.
Semantic interoperability
At this level, systems share a common understanding of data meaning. Standard vocabularies and healthcare interoperability standards, such as SNOMED CT, LOINC, and RxNorm, help you align codes, concepts, and clinical intent. This is critical for analytics, AI, and consistent clinical decision support.
Organizational interoperability
This type focuses on policies, governance, consent, workflows, and agreements. While technology can facilitate data sharing for health care, there is a need for rules, roles, and trust among health care organizations.
Why Interoperability Is Important in Modern Healthcare
The importance of interoperability in healthcare becomes obvious when you connect it to your real goals. You want better outcomes, stronger margins, and sustainable clinician engagement. Fragmented data stands in the way of each of these goals.
Interoperable healthcare systems help you:
- Reduce duplicate tests and procedures by giving clinicians a full view of the patient record.
- Shorten time to insight for quality, safety, and operational metrics.
- Align care across settings so that primary care, specialty, post-acute, and virtual care teams all share the same information.
- Support new types of care models like hospital-at-home and remote monitoring services without requiring one-to-one integration for each service.
Most often, when discussing healthcare interoperability, leaders frame it as a key enabler. Without reliable data sharing in healthcare, clinical transformation, digital engagement, and value-based care programs stall or stay stuck in pilots.
How Interoperability Enables Healthcare Innovation
Healthcare innovation technology depends on trustworthy data flow. You can deploy new tools, but if they sit outside your core systems, you add burden for clinicians and staff. Achieve this through healthcare data interoperability to ensure:
- Enable new digital innovations with minimal disturbance to workflow, since they can be easily integrated with existing infrastructure and data flows.
- Speeding up the test-and-scale process of programs and initiatives, since they can leverage the connections and standards being used instead of having to start building again for each new initiative.
- Collaborative innovation with payers, partners, and startups: Providing access to secure data systems.
- Put insights into action by driving analytics results back into clinical and operational workflows.
Innovation shifts from a series of separate projects to a perpetual state. Its data backbone helps in experimentation and scalability, not limited to the core.
Key Benefits: Connected Care, Efficiency, and Better Outcomes
The importance of healthcare interoperability is most evident in three areas that matter to your teams and your board.
Connected care across settings
Interoperable health care systems enable care journeys that may span multiple settings and organizations. It is possible to share clinical summaries, medication lists, allergy information, imaging reports, and care plans in real time.
This supports
- Safer Transitions of Care.
- More coordinated chronic disease management.
- Better collaboration between primary, specialty, and behavioral health teams.
Operational efficiency and staff experience
When systems exchange and interpret data reliably, you reduce manual chart chasing, duplicate entry, and reconciliation work. Staff get time back to focus on high-value tasks. IT teams manage fewer one-off interfaces and exceptions.
This will directly support retention improvements, reduce burnout risk, and help stabilize operations.
Better clinical and business outcomes
Healthcare data interoperability provides more precise documentation, more timely interventions, and better compliance with best practices. It also facilitates more precise reporting, for example, for contract, quality, and regulatory programs. Such capabilities also improve performance in value-based contracts, strengthen margins, and enhance service line durability.
Role of Interoperability in Digital Health, AI, and Analytics
Digital health tools, AI models, and analytics platforms depend on high-quality, well-structured data. The importance of interoperability in the health sector increases when the capabilities are scaled. Interoperability is helpful in digital health and analytics in different ways.
Reliable inputs for analytics and AI
Such standards will enable you to standardize your data across EHRs, labs, and devices/claims. HL7’s FHIR standard is a significant interoperability standard, important for care coordination, and it entails what it entails. This is a standardized method for accessing clinical and administrative data systems via APIs.
By having a similar structure and meaning, your AI models and analytical pipelines are fed better inputs. This improves model performance, explainability, and trust.
Closed loop insights
Interoperability lets you push insights back into clinical workflows. Predictive risk scores, care gap alerts, and next-best-action prompts appear where clinicians already work, rather than in separate portals.
This turns data sharing in healthcare into action that supports front-line teams and patients in real time.
Integrated digital health tools
When your digital health applications use standardized interfaces and data models, they can plug into your connected healthcare ecosystem. Patient-reported outcomes, remote monitoring data, and digital therapy interactions feed into the record and analytics platforms and then back into care plans.
Interoperability and Patient-Centered Care Models
Patient-centered care depends on a complete, current view of the individual. Fragmented data undercuts that goal. The importance of healthcare interoperability becomes clear when you design care around what patients need rather than what your systems allow.
With interoperable healthcare systems, you can:
- Share visit summaries, medication information, and care plans with patients and caregivers in clear formats.
- Integrate patient-generated data from apps and wearables into clinical decision-making.
- Support shared decision making by presenting a holistic view of history, preferences, and goals.
- Coordinate across organizations so patients experience a single, continuous plan instead of isolated encounters.
Data sharing in healthcare also supports better consent management and privacy controls. You can respect patient choices about where and how data moves while still enabling necessary access for care.
Regulatory Standards and Frameworks Driving Interoperability
Policy, standards, and regulations play a central role in healthcare interoperability importance. They create shared expectations and technical baselines that reduce friction between organizations and vendors.
Healthcare interoperability standards and frameworks influence how you design your architecture and vendor strategy. Key elements include:
- Messaging standards, including HL7 v2, which allow for basic messaging between core systems.
- Document standards that package clinical summaries, imaging reports, and visit information.
- Standards for terminology to align clinical concepts, laboratory tests, and medications.
- HL7 FHIR interoperability profiles and APIs that will support modern application integration, patient access, and partner collaboration.
- Frameworks with respect to information blocking, patient access, and T-E-N.
With these standards and frameworks, your alignment can reduce integration risks, ensure compliance, and prepare your organization for future programs with consistent data exchange.
Challenges and Barriers to Achieving True Interoperability
It is a non-trivial journey, even once standards are set for a particular level of healthcare interoperability. Not only recognizing, but being aware of, these hurdles along the way.
Legacy systems and technical debt
Several core systems were not built to best support modern APIs or rich data models. Integration with digital health tools and other partner platforms must be carefully designed and mapped, sometimes involving modernization or replacement.
Inconsistent data quality and coding
Differences in documentation, coding conventions, and local changes introduce challenges in healthcare data interoperability. You need strong data governance, terminology management, and clinical engagement to reach semantic interoperability.
Vendor and integration complexity
Your environment probably comprises a variety of EHRs, application-specific solutions, and partners, each with their own set of specifications. Managing a varied set of interfaces is a challenge even for sophisticated organizations.
Organizational alignment and governance
However, technical readiness, by itself, is insufficient to convey the importance level of healthcare interoperability that you are seeking. You need shared governance models. They should reach across IT, clinical, regulatory, financial, and operations.
Security and privacy concerns
With the expansion of data sharing in healthcare, there are also more endpoints, users, and use cases. You must coordinate identity, access, consent, and monitoring across systems and partners. Security cannot be an afterthought in an interoperable environment.
Best Practices for Building an Interoperable Healthcare Ecosystem
To fully appreciate the importance of interoperability in healthcare, you need a structured, phased approach. The end goal is to provide a connected healthcare ecosystem that supports current operations and enables innovation going forward.
Practical best practices include:
- Define a clear interoperability strategy. Align on vision, scope, and priority use cases. Tie them to clinical, financial, and operational goals, not only compliance.
- Standardize on core data models and vocabularies. Reduce variation where possible. Develop a reference data model and a terminology standard for all new systems.
- Adopt HL7 FHIR interoperability where it adds value. HL7 informs the use of HL7/FHIR where it adds value. HL7 FHIR-based APIs support external partnerships, patient access, and applications related to digital health
- Invest in integration and data platform capabilities. Interoperability is an enterprise capability, not just a project. Ensure you have scalable integration engines, API gateways, and data platforms.
- Strengthen data governance and stewardship. Ensuring it includes clinical leaders and operational owners. Determining data ownership, quality, and change.
- Focus on user-centered workflows. Design and integration of workflows that assist users and make the job of clinicians and healthcare staff easier. Test and refine.
- Measure value. Track how interoperable healthcare systems affect readmissions, throughput, denials, staffing burden, and patient experience.
Over time, this approach turns interoperability from a reactive integration activity into a core part of your innovation strategy.
Real-World Examples of Interoperability-Driven Innovation
When the importance of healthcare interoperability moves from concept to execution, you see new models of care and operations take shape. Examples include:
- Integrated care coordination. In health organizations, electronic health data is connected to community partners, home healthcare facilities, and post-acute care facilities to facilitate transitions and reduce unnecessary utilization.
- Virtual and hybrid care programs. Remote monitoring technology involves extracting data from a virtual platform and inserting it into the Electronic Health Record and analytics systems. The clinician receives these alerts through their normal workflow.
- Value-based care performance. Payers and providers share data around attribution, quality indicators, and spending trends. A comprehensive perspective enables interventional teams to act earlier.
- Connected specialty networks. Orthopedic, oncology, or cardiology programs use interoperable healthcare systems to share diagnostics, treatment plans, and outcomes across facilities and partner practices.
- Shared analytics environments. Collaboratives and regional networks standardize data through healthcare interoperability standards, then analyze performance trends and equity measures together.
In each case, healthcare data interoperability turns separate systems into a coordinated engine that supports clinical results and strategic growth.
Future Impact of Interoperability on Healthcare Innovation
As technology and policy continue to evolve, the healthcare interoperability importance will only grow. Future models of care and operations will assume seamless data movement.
Trends you should watch include:
- Increased adoption of HL7 FHIR interoperability for near real-time communication, patient-controlled access, and third-party applications.
- More integration between AI and machine learning technology and clinical decisions, operations, and revenues, enabled by standardized data sets.
- Cross-sector sharing, particularly within healthcare, including social services, behavioral health, and community services, following consent and governance.
- Greater expectation from patients with respect to issues like control, transparency, and digital experience.
- Increased regional and national networks that rely on the development of shared healthcare interoperability standards to facilitate coordination.
Organizations that invest now in a healthcare system with interoperability and good data governance will certainly benefit from these developments.
Conclusion
The significance of healthcare interoperability is far from abstract. It shows up in your clinician experience, patient journeys, financial performance, and ability to innovate with confidence.
When you treat interoperability as a strategic capability, not only a technical requirement, you create a connected healthcare ecosystem that supports digital health, AI, advanced analytics, and patient-centered care models. You reduce friction, strengthen trust in data, and create a platform for continuous improvement.
Vorro helps you design and build interoperable healthcare systems that align with your current reality and future goals. Our team specializes in real-world, standards-based integration, HL7 FHIR interoperability, and data sharing across a wide range of health care outcomes.
If you are ready to move from fragmented systems to a coherent, innovation-ready data backbone, schedule a strategy conversation with Vorro.
FAQs
What is the core importance of healthcare interoperability for my organization?
The core importance of interoperability in healthcare is that it turns isolated systems into a connected platform for care, operations, and innovation. It provides your teams with reliable, timely access to the data they need, reduces manual work, and improves clinical and financial outcomes.
How do healthcare interoperability standards support innovation?
Healthcare interoperability standards create common formats, vocabularies, and interfaces that reduce integration effort and risk. When your systems align with standards such as HL7 and HL7 FHIR interoperability profiles, you can introduce new tools, partners, and programs more quickly without rebuilding your data plumbing each time.
What is the difference between data integration and healthcare data interoperability?
Data integration focuses on moving data between systems. Healthcare data interoperability goes further. It ensures that data is structured, coded, and governed in ways that preserve meaning and support use in workflows, analytics, and decision support across multiple systems and organizations.
How do I know if my current systems are interoperable?
You can assess interoperability in healthcare systems by examining how easily data flows between them, how often staff perform manual workarounds, and how well different applications interpret shared data. Formal assessments may be conducted to verify interfaces, standards used, data quality, and alignment with healthcare interoperability standards.
Where should I start if my organization has many legacy systems?
Begin with a well-defined strategy based on high-value use cases such as transitions of care, readmission reduction, value-based performance, and more. Follow this with the development of your integration and data strategy, based on standards such as HL7 FHIR, where applicable, and the normalization of existing legacy systems. Working with an interoperability specialist can help you take steps in a controlled, measurable way.
The firm Vorro has extensive expertise in integration, data interoperability in health care, and connected or interoperable health care ecosystems, which can help you move away from point-to-point fixes toward a sustainable approach to interoperability that supports long-term health care innovation technologies.
Akshita is a Senior Content Writer and Marketer with over a decade of experience crafting narratives that convert, rank, and build lasting brand authority. She has worked across SaaS, FinTech, HealthTech, and Education spaces, delivering everything from HIPAA-compliant medical content to multilingual campaigns for the International Labour Organization, United Nations. Her content has reached audiences across the globe, and she has worked for Fortune 500 brands, global agencies, and startups alike. Fluent in English, Spanish, and German, Akshita brings a rare cross-cultural edge to brand communication. A literature graduate from Delhi University, she balances strategic thinking with a storyteller's instinct, but when she isn’t architecting content roadmaps, she channels her creativity into poetry and painting or dedicates her time to caring for stray animals - pursuits she credits for making her a more empathetic and perceptive communicator.