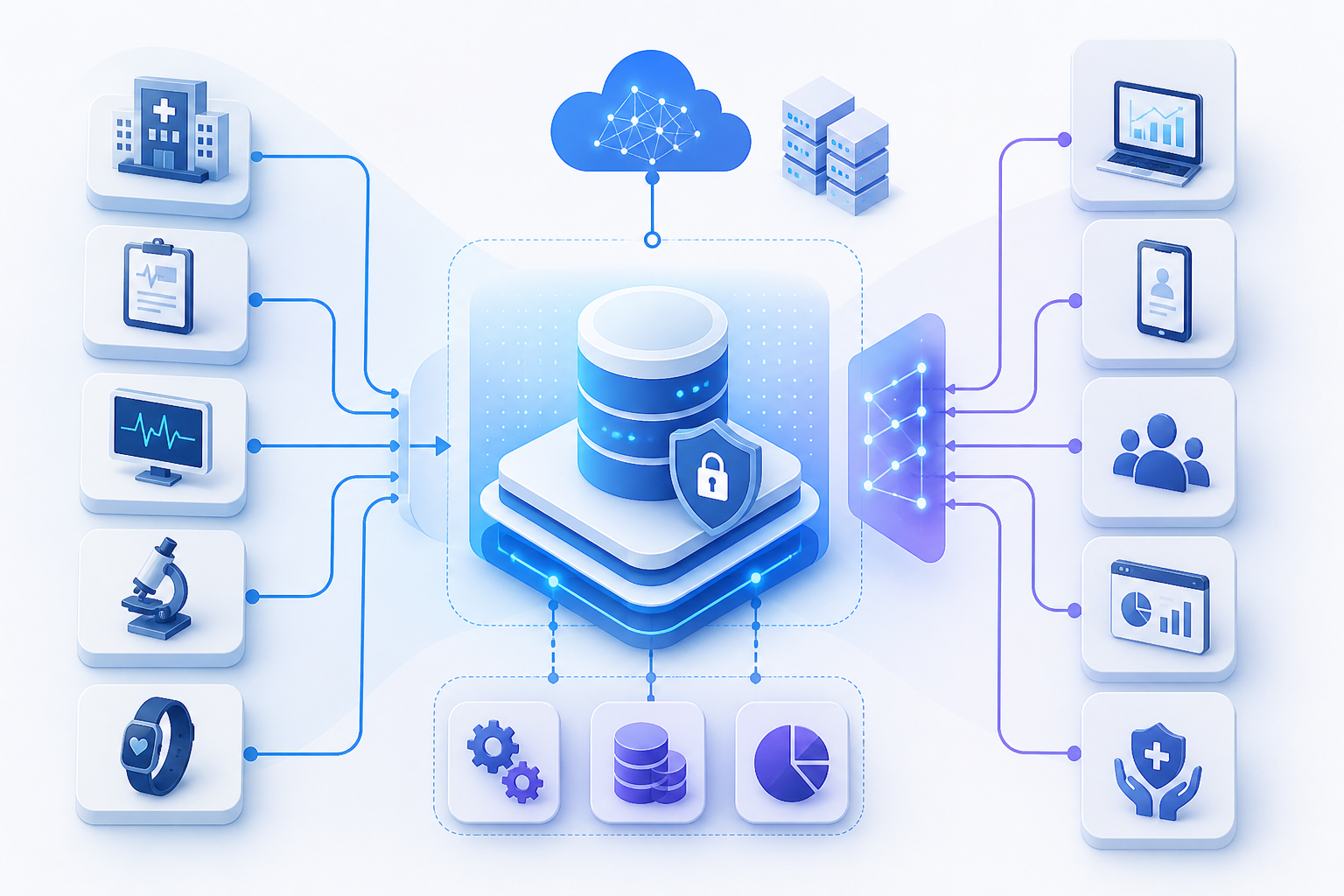
Throughout history, no one has ever had access to as much clinical and operational data as you do now in your organization. But when looking for a single source of truth across EHRs, HIEs, revenue cycle tools, CRM platforms, and partner systems, you usually find discrepancies, workarounds, and delays in your initiatives.
This is the core issue of cross-system healthcare data governance. You are not struggling because you have insufficient data. You are struggling because you have no unified, governed method to control how data is flowing, changing, and being trusted across systems and partners.
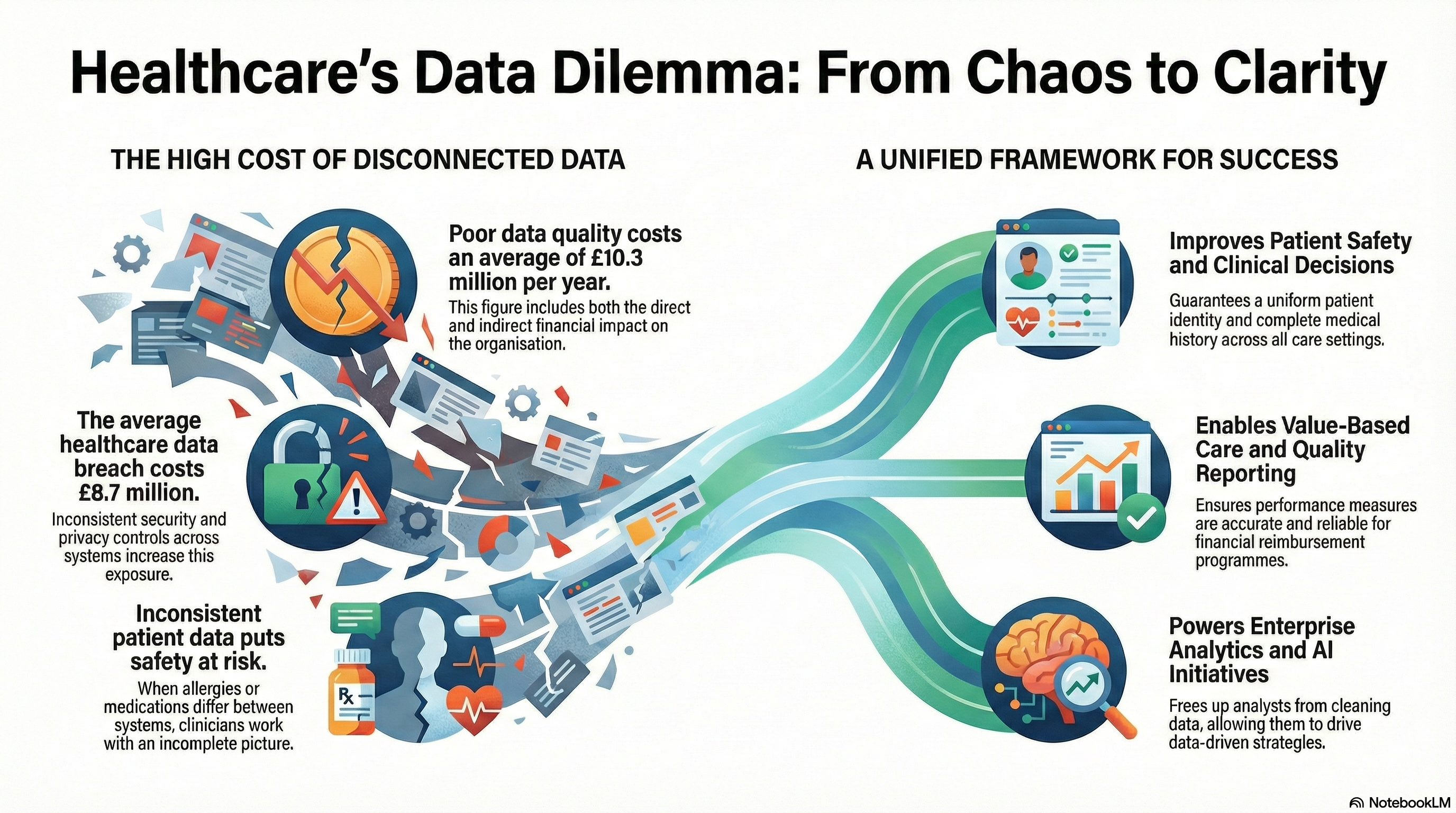
The stakes are getting higher and higher. One study revealed that poor data quality costs organizations, on average, $12.9 million a year in both direct and indirect impact. Another report claims that as much as 30 percent of the global healthcare expenditure is waste, a large part of which is caused by administrative complexity and information gaps.
If you want your analytics, care coordination, and patient experience strategies to be successful, you need to figure out the reasons behind cross-system governance being so difficult and what needs to be done to solve it.
What Is Healthcare Data Governance
Healthcare data governance is the department that specifies the ways in which your organization handles and exploits data as an asset. It establishes policies, decision rights, and controls that specify how data is:
- Defined and standardized across clinical, financial, and operational domains
- Collected, validated, and corrected
- Secured and accessed under HIPAA and other regulations
- Shared across departments, partners, and digital channels
- Used for reporting, analytics, and automation
A healthcare data governance framework typically encompasses different layers, such as:
- Strategy: Explain the role of data in achieving your clinical and business goals
- People: Data owners, stewards, and governance councils
- Policies: Naming standards, quality rules, retention, access, and sharing
- Processes: How data is onboarded, integrated, corrected, and monitored
- Technology: Integration, MDM, metadata, and monitoring platforms
If a framework is running perfectly, your employees will be able to speak the same data language. Your quality measures will be consistent with your claims data. Your clinical teams will have enough trust in the reports to change work processes accordingly. Your IT teams will be able to avoid custom one-off integrations that break every time a vendor updates a schema.
Most organizations do some of this inside a single system or domain. The struggle begins when you extend those practices across systems, vendors, and external networks.
What Is Cross-System Data Governance
In healthcare, cross-system data governance extends the essence of core governance practices to all systems and endpoints that are involved with your data. It recognizes data as a shared asset among:
- Different instances and versions of EHRs
- Specialty or departmental systems
- Revenue cycle, CRM, and contact center platforms
- HIEs, payer portals, and external registries
- Telehealth, patient engagement, and eCommerce solutions
Rather than controlling data within each application, you set the rules at the enterprise level. The rules are with the data wherever it goes. That includes:
- How do you identify a person or provider across systems
- How do you standardize codes, terminologies, and reference data
- How you manage consent and privacy flags beyond a single EHR
- How do you propagate corrections and updates across downstream systems
- How do you audit who touched what data and where
With cross-system healthcare data governance, you link together the dots between your source systems and the way care is delivered, documented, billed, and measured. It is at the conjunction of integration, interoperability, security, and analytics.
Why Cross-System Governance Is Critical in Healthcare
You already notice the effect of disorganized data on your daily work. When governance is stretched across different systems, it not only reveals pain points but also turns them into measurable enterprise risks and missed opportunities.
-
Clinical decision support and patient safety
When patient allergies, medications, or problem lists are not the same across different systems, doctors only get a partial picture. According to research published in the JAMA Network, safety events related to electronic health records (EHR), especially those leading to medication ordering errors and clinical decision support issues, are still very common, and they are mainly due to information gaps and inconsistencies between systems.
Healthcare data governance that is consistent across systems. It guarantees uniform patient identity, code sets, and documentation standards. Thus, the scenario of a clinician being unaware of a vital history because it is stored in a disconnected system, and the clinician is working on an incomplete record, is less likely to happen.
2. Value-based care and quality reporting
Quality measures gather data from various sources such as EHRs, claims, registries, and patient-reported outcomes. Your measures will vary, and your performance will appear unreliable if each system defines and codes data differently.
CMS programs are constantly linking money to being able to provide data reporting that is both accurate and timely. Just in 2023, the Medicare Shared Savings Program took care of 482 ACOs and 13.7 million beneficiaries, and each ACO is dependent on cross-system data aggregation and governance for performance measurement.
3. Digital front door and patient experience
Patients expect to get the same information no matter where they are scheduling sessions, logging in to their portals, looking at their bills, or being engaged on the different platforms. In case there are demographic updates, consent preferences, or insurance coverage information differences between the systems, the patients will lose trust, and the number of calls will increase.
Cross, system governance makes it possible that a change in the patient phone number, a choice to get SMS reminders, or a change of PCP made through one channel automatically and correctly reflects in your entire ecosystem.
4. Enterprise analytics and AI initiatives
Analytics and AI projects rely heavily on accurate and properly managed data. According to a survey conducted by NewVantage Partners, only 26 percent of companies have been able to transform into data-driven organizations, with data quality and silos being the main problems.
Your analytics team, without cross-system governance, is stuck with the majority of its time cleaning and reconciling data coming from different feeds. That slows down the strategic work and increases the risk that executives make decisions on inconsistent numbers.
5. Regulatory compliance and security
HIPAA, state privacy laws, and contracts with payers and partners require consistent control over PHI, no matter which system contains the information. If consent flags or privacy restrictions are only kept inside the EHR, you run the risk of not complying with the patient’s preferences in other channels.
Robust cross-system governance integrates consent, access control, and audit features throughout the entire integration footprint, even including external exchanges and digital front ends.
Key Challenges Healthcare Organizations Face
If cross-system healthcare data governance is so important, why are there so many healthcare organizations that still have trouble with it? Several recurring healthcare data governance challenges can be seen in health systems, payers, and health IT vendors.
1. Fragmented ownership and accountability
Data ownership is frequently divided among clinical departments, IT, analytics, finance, and compliance. Each group focuses on its own priorities and tools. No one takes responsibility for the entire data lifecycle from source to consumption, especially when it comes to crossing systems.
When there are no definite data owners and stewards, your governance policies remain only as documents. Special cases become the norm, and inconsistent definitions quietly spread to new integrations and reports.
2. Multiple vendors and integration patterns
Basically, a health system will have several EHRs, a few specialty tools, and an increasing number of cloud applications. Each vendor has their own data model, integration options, and upgrade path. After a while, there are many point-to-point integrations.
Then your team handles hundreds of customized mappings, transformations, and interface issues. Every change request presents a risk of disrupting downstream flows. Governance policies seldom manage to keep up with this speed and variety.
3. Legacy systems and technical debt
Lots of core systems were installed long before your current analytics and interoperability needs. They still hold vital data using proprietary formats or custom fields. Documentation is either not available or is outdated.
Adding new APIs, FHIR servers, and cloud analytics as a layer on top, you get inconsistent data types, old code sets, and local workarounds along with the inherited data. These problems will be part of your integration logic unless governance steps in.
4. Inconsistent data definitions and standards
Even in one healthcare organization, various departments will have their definitions for the terms encounter, visit, or active patient. Different systems use different code sets and value lists. Some terminologies like SNOMED CT, LOINC, and RxNorm might be only partially implemented, or usage might be inconsistent.
These inconsistencies rank among the most intractable healthcare data governance problems. They come up whenever you attempt to compare site performances, compile registries, or match clinical events with claims.
5. Manual processes and local workarounds
When data quality issues obstruct their work, employees start to improvise. They come up with spreadsheets, local databases, or even add custom fields in their applications. They re-enter data manually between systems if the interfaces do not work. These temporary solutions circumvent the formal governance system and are hardly ever documented. They actually increase the level of risk, and on top of that, they inject even more variation into the data lifecycle, thus making future integrations that much more difficult.
6. Limited visibility across the full data flow
A lot of teams do not have a clear picture of data movement from the source to the endpoint. Lineage, usage patterns, and quality metrics are kept in different tools, if at all. Without an enterprise-wide overview, enterprise healthcare data governance turns into a reactive approach. It is only after billing, clinical operations, or compliance have been affected that you learn about the issues.
Impact of Poor Data Governance
Poor cross-system healthcare data governance can be broadly understood as inefficient management of healthcare data that is spread across different systems or platforms. The problem is often manifested as long registration lines, fragmented portals, and doctors who do not use decision support tools because they distrust the data.
Besides the obvious operational inefficiencies and patient dissatisfaction, poor governance of healthcare data that is shared across different systems not only creates IT headaches but also directly affects financial performance, clinical quality, and strategic flexibility.
1. Financial leakage and administrative waste
The Council for Affordable Quality Healthcare (CAQH) published a report estimating potential annual savings of $25 billion in the healthcare industry through automation and standardization of administrative transactions, many of which rely on clean, well-governed data.
2. Patient and provider experience erosion
When patients have to give their information several times, or they get different directions from different people, their trust gradually diminishes. When doctors have to use time to fix records and doubt the reports, their exhaustion rises, and the implementation of new tools gets delayed.
3. Compliance and security exposure
Unaligned consent, lack of complete recording of the audit, and different roles, based on access between the systems, make your risk profile higher. A single connection that does not take updated privacy rules into account can give unauthorized users access to PHI.
Data breaches stay costly. IBM’s 2023 report revealed that the average cost of a healthcare data breach hit $10.93 million, the highest among all sectors. Although breaches are incidents involving numerous factors, ill management of the systems’ governance is often a contributing factor in why the cases become difficult to contain and remediate.
4. Slower innovation and missed opportunities
Each new program, partnership, or digital product is reliant on the integration of data across boundaries. If a strong healthcare data governance framework is lacking, then each initiative is turned into a custom integration with new rules and exceptions.
Executives delay the implementation of new analytics, automation, or patient experience solutions because of data issues discovered during previous attempts. Your development plan slows down while competitors with stronger enterprise healthcare data governance are able to move at a quicker pace.
5. Low trust in the analytics and reporting
When already high-ranking officials question the source upon seeing diligence in reports based on different sets of data. Various teams dedicate their meetings to arguing over the accuracy of data rather than addressing issues. Data analysts spend most of their days clarifying terms and aligning datasets. Gradually, it is losing its perceived value of data and analytics that are the basis of your investments. Decision-making, which is of great worth, gradually loses its focus on centralized insights and goes back to local anecdotes and spreadsheets.
Conclusion
Cross-system healthcare data governance is not something that can be left for later. It is the very base that ensures your quality programs, digital front door, enterprise analytics, and compliance posture can function effectively.
To progress, a single policy document won’t suffice. You require:
- A strong backing from top management and data being recognized as a shared enterprise asset between them, with a focus on accountability
- Data ownership, domain, and system-based stewardship are clearly communicated and understood roles
- Uniform definitions, code sets, and quality rules that are harmonized across the whole ecosystem
- Integration and interoperability platforms that are capable of enforcing the governance as the rule and not the exception
- Continuous data quality, lineage, and usage are being tracked across all endpoints.
From the inside, such organizations are pretty much the same ones co, sharing the complexities of the healthcare system with their stakeholders, only that they no longer allow those complexities to dictate the use of data in their line of work. What they essentially do is set up a kind of rhythm in which they are able to keep introducing new systems, establishing partnerships with payers and community providers, and ensuring the delivery of consistent patient experiences.
Vorro supports health systems, payers, and health IT vendors in resolving healthcare data governance issues across different systems at the integration layer. Our integration and interoperability solutions unravel complex data flows, establish a uniform method of data exchange between systems, and facilitate the implementation of healthcare data governance best practices across your enterprise.
If you are looking to diminish healthcare data governance challenges, enhance your enterprise healthcare data governance program, and turn your healthcare data governance framework into a long-lasting one, get in touch with Vorro regarding your integration and governance strategy.
FAQs
What is cross-system healthcare data governance?
Cross-system healthcare data governance refers to a collection of policies, roles, and controls that guarantee consistent, secure, and high-quality data not only to your systems, but to all vendors and partners in your ecosystem. It is mainly concerned with how data flows from one system to another and how, along the route, definitions, quality rules, and privacy controls remain consistent.
How is cross-system data governance different from basic data governance?
Basic governance is commonly limited to data inside a single system or domain, for instance, an EHR or a data warehouse. Cross, system governance takes those practices and applies them to every application and integration in the organization. It tackles issues such as patient identity being the same across systems, the use of consistent code sets, cross, application consent, and end, to, end lineage from source to consumption.
What are the most common healthcare data governance challenges?
There is fragmented data ownership where different teams or departments each think they own their data and refuse to share or cooperate. Also, MR systems, medications, laboratory, billing, etc., vendors may have different data models, causing inconsistent data. Sometimes old systems (legacy) restrict digital transformation efforts by not supporting new features or standards. The definitions and standards used are never the same across departments, units, or partners. Business processes that are automated most of the time are occasionally done manually, resulting in human errors. Not having complete visibility of how data flows from one system to another complicates matters. All these factors lead to the fact that it is very difficult to maintain quality, consistency, and compliance as data moves.
Why do health systems struggle with enterprise healthcare data governance?
Typically, one major reason is that, in the past, the focus of investment was on the applications, i.e., the single software piece, rather than looking at the enterprise data holistically. Solutions such as standard operating procedures for data may be there, but due to a lack of empowerment, they cannot be truly effective across various departments and vendors. Integration teams are the ones who suffer the most as they have to resolve the differences without a unified, shared governance framework that guides them to make decisions and follow standards.
What are healthcare data governance best practices for cross-system environments?
First and foremost, executive support is crucial for data governance activities as they are fundamental and ever-present. Another crucial element is clear data ownership and stewardship. Along with that, there is a need to agree on data definitions and code sets, which should be standardized throughout the organization. Moreover, central management of identity and consent, using integration platforms that consistently implement governance rules, continuous data quality, and lineage monitoring are the main point. Furthermore, working with experienced integration providers such as Vorro can be a very valuable channel for converting strategies into working solutions.
Akshita is a Senior Content Writer and Marketer with over a decade of experience crafting narratives that convert, rank, and build lasting brand authority. She has worked across SaaS, FinTech, HealthTech, and Education spaces, delivering everything from HIPAA-compliant medical content to multilingual campaigns for the International Labour Organization, United Nations. Her content has reached audiences across the globe, and she has worked for Fortune 500 brands, global agencies, and startups alike. Fluent in English, Spanish, and German, Akshita brings a rare cross-cultural edge to brand communication. A literature graduate from Delhi University, she balances strategic thinking with a storyteller's instinct, but when she isn’t architecting content roadmaps, she channels her creativity into poetry and painting or dedicates her time to caring for stray animals - pursuits she credits for making her a more empathetic and perceptive communicator.