By Anubhav Awasthi · February 7, 2026
You feel pressure from every direction. You need better clinical insight, cleaner reporting, and stronger financial performance. You invest in analytics tools, dashboards, and reports, yet you still do not trust the data. The root problem sits underneath the dashboards. Your data is not integrated.
Healthcare analytics data integration is the quiet work that determines whether your analytics efforts deliver value or drain time. Without it, your organization runs on partial truths. With it, you create a healthcare analytics data foundation that supports clinical, operational, and financial decisions at scale.
If you lead data, analytics, IT, or operations in a provider, payer, or health tech organization, your analytics outcomes depend on how you treat integrated healthcare data. The technology matters, but your approach to integration matters more.
What Is Integrated Data in Healthcare
Integrated healthcare data is a consistent, unified view of patient, clinical, financial, and operational information across systems. It connects data from EHRs, practice management, billing, labs, imaging, CRM, care management tools, and digital front door solutions into a single, trusted layer.
Healthcare analytics data integration focuses on how you move, align, and standardize this data so analytics teams can work with a coherent picture. Instead of treating each system as an island, you create an ecosystem where data flows in a controlled, governed way.
At a practical level, integrated healthcare data means:
• Linking patient identities across multiple source systems into one master record
• Standardizing codes and values so you can compare and aggregate information
• Transforming source data into consistent models that analytics tools understand
• Managing data flows in real time or near real time, not only through nightly batches
Clinical analytics data integration focuses on clinically relevant sources, such as EHR data, lab results, imaging metadata, pharmacy fills, care plans, and device feeds. When you integrate these sources properly, you stop guessing about the patient story and start seeing it in one view.
Why Integrated Data Is the Foundation of Healthcare Analytics
Every analytics ambition depends on the stability of your healthcare analytics data foundation. If your data is fragmented, inconsistent, or stale, your analytics will reflect those weaknesses, no matter how advanced the tools or models.
Healthcare analytics data integration creates this foundation. It gives you:
• A single trusted source for key metrics instead of multiple conflicting reports
• Shared definitions of measures across clinical, financial, and operational teams
• Clear ownership and governance for how data flows and who can use it
Healthcare analytics integration also bridges the gap between IT and business teams. IT focuses on secure, reliable pipelines. Business teams focus on decisions. Integration connects these priorities so you move faster, with fewer disputes about whose numbers are correct.
Without an integrated foundation, every new analytics request feels like a custom project. With strong healthcare analytics data integration, each new question plugs into a consistent, reusable set of data and models. Your team spends less time wrangling and more time analyzing.
Challenges of Healthcare Analytics Without Data Integration
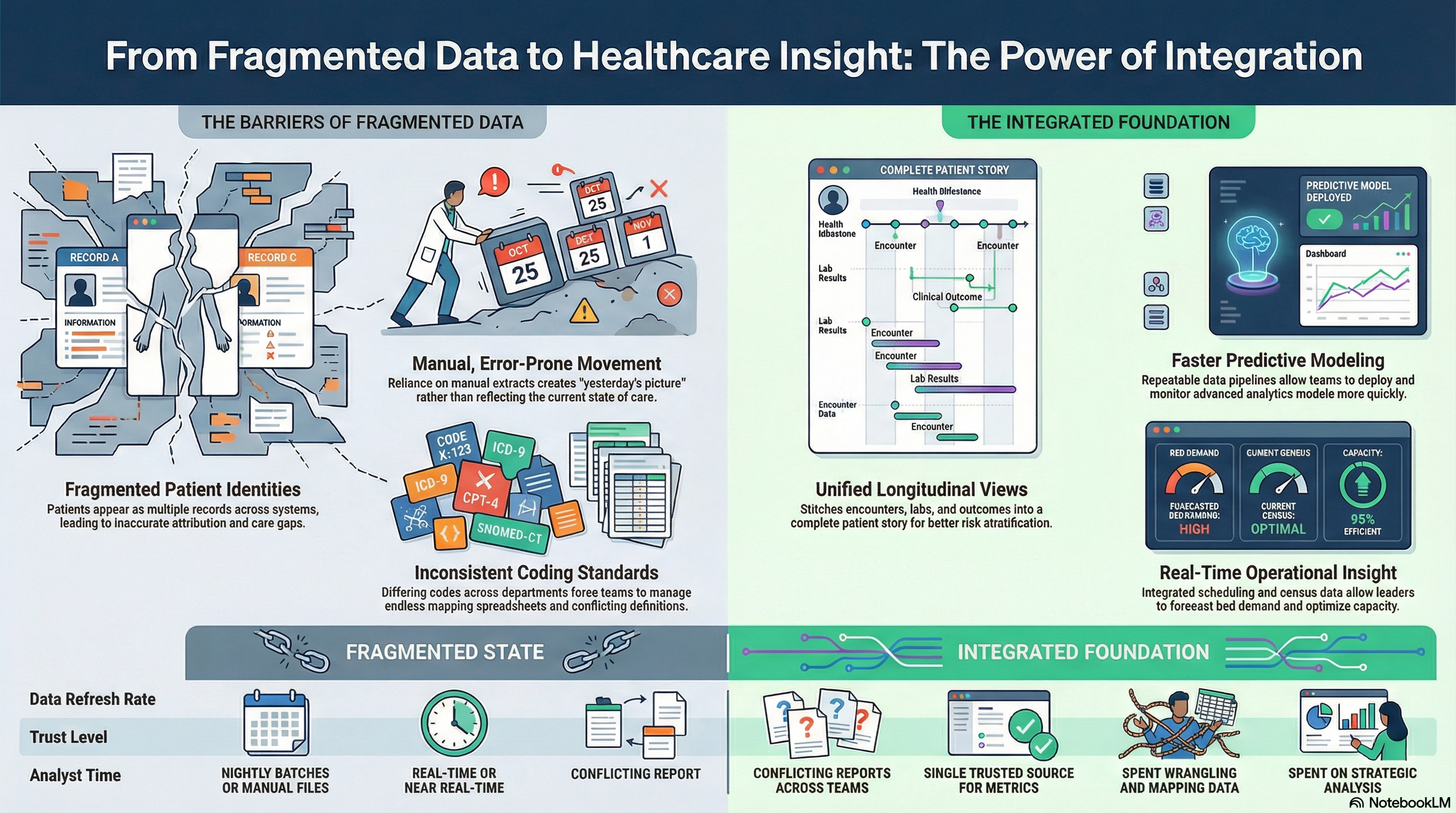
If you rely on disconnected systems and manual extracts, your analytics program faces consistent barriers. These challenges slow every initiative, from operational dashboards to advanced clinical analytics.
Fragmented Patient and Provider Identities
Without integrated healthcare data, the same patient appears as multiple records across systems. The same provider or facility appears with different identifiers. Analytics teams spend time reconciling data instead of analyzing it. This fragmentation leads to inaccurate attribution, gaps in care histories, and flawed outcomes analysis.
Inconsistent Coding and Data Definitions
Each system follows its own coding and documentation practices. Diagnosis codes, procedure codes, units, and statuses differ. Without healthcare analytics data integration, your team manages endless mapping spreadsheets and fragile logic in reports. You end up with contradictory definitions of quality, cost, and performance across departments.
Manual, Error-Prone Data Movement
Teams download flat files, upload them to analytics tools, and maintain one-off transformations. This manual work introduces errors and version confusion. It also limits the frequency of updates. Your analytics reflects yesterday’s or last week’s picture, not the current state of care.
Limited Use of Clinical Context
When clinical analytics data integration is weak, clinical context sits locked in EHRs, unstructured notes, and siloed registries. Analysts lean on billing or claims data, which omits the nuance of clinical care. Advanced models underperform because they lack a rich clinical signal.
Hidden Compliance and Security Risk
Uncontrolled data sharing and manual extracts increase privacy and security risk. Without a defined healthcare analytics integration strategy, PHI moves unpredictably across teams and tools. Logging, access control, and auditing become hard to manage.
How Data Integration Enables Advanced Healthcare Analytics
Once you treat healthcare analytics data integration as a strategic capability, your organization unlocks new types of analysis and decision support. Integration shifts analytics from reactive reporting to proactive intelligence.
Unified, Longitudinal Patient Views
Integrated healthcare data enables a longitudinal patient record that stitches together encounters, lab results, medications, referrals, and outcomes. This record supports risk stratification, care gap identification, and population health programs. Analysts work from a complete story instead of scattered snapshots.
Richer Clinical Analytics Pipelines
Clinical analytics data integration connects structured and semi-structured clinical data with operational and financial sources. You can:
• Analyze care variation by combining order sets, outcomes, and cost
• Support clinical decision support models with timely lab and vitals data
• Evaluate new care pathways with reliable before and after comparisons
Timely Operational and Financial Insight
Stable healthcare analytics integration delivers near real time feeds of scheduling, census, capacity, and revenue data. Operations leaders make resourcing decisions based on what is happening now, not historical reports. Revenue cycle teams monitor denials, AR trends, and payer behavior with fewer delays.
Faster Deployment of Advanced Models
If your analytics team wants to introduce predictive or prescriptive models, healthcare data integration for analytics becomes essential. Models depend on consistent inputs and repeatable pipelines. With an integrated foundation, you can:
• Deploy models into production workflows more quickly
• Monitor model performance with consistent feature definitions
• Reduce rework when you adjust or replace models
Stronger Governance and Data Trust
Integration gives you a central place to enforce quality checks, access controls, and logging. Analysts and business leaders gain confidence that metrics are calculated the same way across tools and departments. This trust raises adoption of analytics and reduces time spent debating numbers.
Key Benefits for Healthcare Organizations
When you stabilize your healthcare analytics data foundation, tangible benefits follow across the organization. Integration supports a more coordinated approach to clinical care, operations, and finance.
Better Clinical Decision Support
With integrated healthcare data, clinicians and care teams receive insights based on full histories, current clinical indicators, and social determinants, not incomplete views from a single system. Clinical analytics data integration helps identify high-risk patients earlier and supports earlier interventions.
More Effective Population Health Programs
Population health teams depend on healthcare data integration for analytics across EHRs, registries, and claims. Integrated data helps you:
• Define target cohorts accurately
• Track care gaps and outreach in a consistent way
• Measure outcomes and program impact with confidence
Stronger Financial Performance and Contract Management
Integrated financial, clinical, and claims data supports value based care contracts, bundled payments, and payer negotiations. Healthcare analytics integration enables clear insight into utilization patterns, cost of care, and performance against contract terms. Finance teams gain a more reliable base for strategic planning.
Improved Operational Efficiency
Operations leaders gain a cohesive view of throughput, staffing, resource use, and patient flow. Instead of piecing together metrics from separate sources, they see how decisions in one department affect others. This integrated perspective supports more agile capacity management and resource allocation.
Reduced IT and Analytics Friction
When healthcare analytics data integration is robust, IT teams manage fewer one-off data requests. Analysts reuse shared datasets and views. New projects stand up faster because the core integration work already exists. This reduces burnout and helps you attract and retain analytics talent.
Real-World Healthcare Analytics Use Cases
Strong integration supports practical, high impact use cases across provider, payer, and health tech organizations. These examples show how healthcare analytics data integration underpins both strategic and tactical work.
Reducing Avoidable Hospital Utilization
A health system wants to reduce avoidable emergency visits and readmissions. With integrated healthcare data, the team:
• Combines EHR, claims, and social data into risk scores
• Flags patients at high risk and routes them to care management
• Tracks interventions, follow up visits, and outcomes in one system
Without healthcare analytics data integration, this program would rely on manual lists, partial data, and delayed feedback.
Supporting Value Based Care Performance
An accountable care organization manages multiple payer contracts. Healthcare data integration for analytics aligns claims, eligibility, EHR data, and quality measures. Analytics teams:
• Monitor attribution and panel changes continuously
• Track quality gaps at patient and provider levels
• Analyze cost drivers across conditions and service lines
This integrated approach supports stronger negotiations and better performance against contract targets.
Optimizing Operating Room and Bed Capacity
A hospital wants to improve throughput and reduce delays. With healthcare analytics integration across scheduling, EHR, perioperative systems, and bed management, teams:
• Forecast demand by service line and time of day
• Identify bottlenecks tied to specific resources or processes
• Coordinate staffing and scheduling based on data, not anecdote
Enhancing Patient Engagement and Digital Front Door
An integrated delivery network runs digital front door tools, call centers, and CRM platforms. Integrated healthcare data connects digital engagement, clinical records, and contact preferences. The organization:
• Targets outreach based on clinical need and engagement history
• Aligns communication across channels for a consistent experience
• Measures the effect of engagement strategies on outcomes and utilization
Supporting Clinical Research and Innovation
For research teams, clinical analytics data integration across EHR, imaging, and registries supports cohort selection and outcomes tracking. When integration is strong, you:
• Identify eligible participants more quickly
• Follow outcomes across care settings with less manual chart review
• Share de-identified data with partners in a controlled way
Conclusion
Healthcare analytics data integration is not an optional technical project. It is the core capability that shapes every decision your organization makes from the bedside to the boardroom. Without an integrated healthcare analytics data foundation, you will continue to face conflicting reports, manual work, and limited impact from analytics investments.
With the right integration strategy, you create a reliable, scalable base for clinical analytics data integration, operational insight, and financial performance. You support your teams with timely, trusted information instead of manual workarounds. You turn data into a practical asset that advances your mission.
Vorro focuses on healthcare analytics integration that respects your existing systems, reduces complexity, and delivers a stable data foundation for your teams. If you want to strengthen healthcare data integration for analytics and move your organization toward confident, data driven decisions, schedule time with Vorro to talk about your integration roadmap.
FAQs
What is healthcare analytics data integration?
Healthcare analytics data integration is the process of connecting, standardizing, and governing data from multiple healthcare systems so analytics teams can work from a single, trusted source. It aligns clinical, financial, operational, and patient data in a consistent way for reporting, dashboards, and advanced analytics.
Why does integrated healthcare data matter for analytics?
Integrated healthcare data removes conflicting numbers, manual reconciliations, and blind spots in patient and provider information. It lets you answer questions with confidence because all teams rely on the same definitions and shared datasets. This foundation is critical for accurate reporting, quality programs, and value based care.
How is clinical analytics data integration different from general integration?
Clinical analytics data integration focuses on clinically rich sources, such as EHR data, labs, imaging, and care plans, and links them with outcomes and utilization. It prioritizes context that supports care decisions, risk models, and quality measures, not only financial or operational metrics.
What should healthcare organizations look for in a data integration partner?
You should look for deep healthcare experience, proven interoperability capabilities, strong security and compliance practices, and a clear integration roadmap. The partner should understand your clinical and business goals, not only your technical stack, and should help you create a sustainable healthcare analytics data foundation.
How does Vorro support healthcare analytics integration?
Vorro focuses on healthcare analytics data integration for providers, payers, and health tech organizations. The team connects complex systems, standardizes data, and supports governance so you can trust your analytics across clinical, operational, and financial domains. Vorro aligns integration work with your strategic goals and existing technology.
Vorro helps healthcare organizations treat integrated data as a strategic asset, not a side project. To see how Vorro can support your integration strategy and analytics priorities, visit Vorro.












