By Akshita Kohli · February 14, 2026
Population health initiatives frequently come to a halt when patient data remains in isolated databases. Healthcare, insurance, social, and administrative data are stored in separate systems, with separate formats, and separate owners. You experience the effects in each of your programs. Care gaps remain undiscovered. Risk predictions become inaccurate. Communication campaigns become less targeted. Staff do not have a common reference point. The combination of data for population health management changes those isolated sources into one, a single, usable asset that facilitates better decisions, better collaboration, and better population health outcomes.
What Is Integrated Data in Healthcare
Integrated data in healthcare is when you combine data from various clinical, financial, and operational systems into one unified, consistent view. Instead of having to log into multiple tools and download different spreadsheets, you can just use one single, trusted source that gathers everything in a neat and well, managed structure.
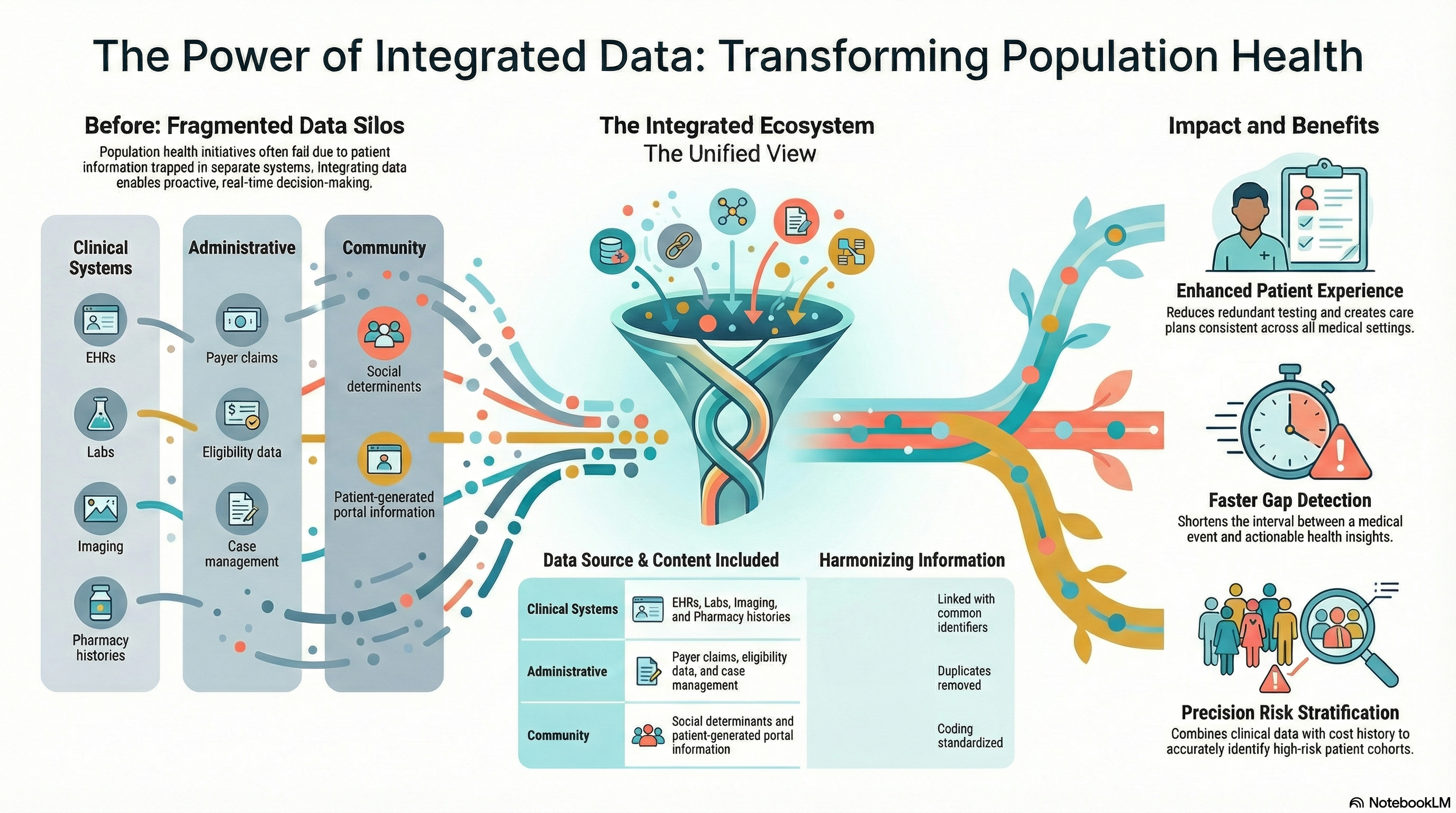
Integrated data for population health management is a wide, ranging initiative covering all the aspects that influence risk and outcomes. Generally, it includes:
- Electronic health records from hospitals, clinics, and specialty providers
- Claims and eligibility data from payers
- Pharmacy and medication histories
- Lab, imaging, and diagnostic systems
- Care management and case management platforms
- Social determinants and community resources data
- Patient generated information from portals and remote monitoring tools
Population health data integration links the various sources through common identifiers and shared definitions. It finds and removes duplicate records, converts codes to a standard, and synchronizes updates. In this way, you can get the whole picture of an individual, a group, or a community without having to reconcile manually each time you want to take action.
Robust clinical data integration for population health not only manages to understand workflow but also establishes the connection to the systems used by clinicians and care teams for their daily work. This prevents integrated data from becoming “siloed” and, furthermore, it is able to support actual decisions, not only retrospective reporting.
Overview of Population Health Management
Population health management is about enhancing the care outcomes and experience of specific groups of people in a cost-efficient manner. You don’t isolate a single visit but rather coordinate care, patient engagement, and resource allocation throughout the entire lifecycle of your population.
Some of the widely shared population health goals are:
- Lowering unnecessary hospital stays and readmissions
- Enhancing the management of chronic diseases within cohorts
- Boosting quality measures performance under value-based contracts
- Allocating resources to people at rising or high risk
- Dealing with gaps related to access, equity, and social needs
To accomplish these objectives, robust healthcare data integration for population health that links individuals, processes, and technology is necessary. Typically, such work goes over:
- Risk stratification and predictive models
- Care coordination workflows and pathways
- Patient engagement and communication programs
- Performance monitoring and continuous improvement
- Collaboration with payers, community partners, and public agencies
Population health analytics backed by integrated data is the focal point of such a strategy. It provides executives, healthcare providers, and data experts with a common basis for making decisions about what to concentrate on, whom to involve, and how to measure the effects.
Why Integrated Data Is Critical for Population Health
You are unable to control what you do not have a clear view of. Integrated data for population health management provides you with the transparency that you require no matter the setting of the care, the contracts, or the communities. Population health, however, becomes a puzzle with pieces from only a few insights without it.
Listed below are some of the fundamental reasons why integrated data is essential.
Whole person visibility
Patients are not only moving between care sites but also between networks. Moreover, they utilize community services and digital tools. The integration of population health data links all these interactions into a single longitudinal track. You are able to view diagnoses, procedures, medications, labs, behavioral health, and social needs all together, rather than seeing them as separate events.
Stronger risk and stratification models
If you supply risk models with only claims data or only EHR data, you will miss out on patterns. Integration of clinical data for population health combines detailed clinical information with cost and utilization history. This enhances the accuracy of cohort definitions, risk tiers, and care pathways, resulting in more accurate targeting of interventions.
Faster detection of gaps and trends
Population health analytics with integrated data greatly shortens the interval between an event and the insight gained from that event. Without the need to wait for periodic reports, you can follow the increase in risk, care gaps, and quality performance almost immediately. This accelerates decision, making and gives the opportunity for remedy to be done before the problems become serious.
Alignment across stakeholders
Various teams are using different tools, but population health still necessitates a common understanding at the very least. Healthcare data integration for population health offers payers, providers, and partners, among others, stable metrics and definitions. This thus diminishes the obstacles that exists, increases the cooperation between the parties and facilitates the joint planning.
How Integrated Data Supports Population Health Initiatives
Integrated data for population health management is not just a concept. It becomes evident in everyday work across projects. If you bring data and workflows into alignment, each program becomes more clear and accurate.
Targeted outreach and engagement
Integrated data enables you to pinpoint individuals who require outreach from the complete set of clinical and social signals. you can:
- Detect the vulnerable patients even before they become very costly patients
- Find out the patients who have not attended the follow, up or do not have preventive care
- Make a breakdown of the groups according to language, communication preference, or social issues
Population health data integration is a great support for timely and correct outreach lists. Case managers and outreach teams spend much less time on manual searching and more time talking to the right people.
Care coordination and transitions
Patient care transitions will be subject to a high level of risk if the patient’s information is not transferred with them. Clinical data integration for population health involves discharge plans, medication lists, and follow, up instructions being fed to primary care, specialists, and community partners via the tools that they use. That:
- Reduces duplicate tests and conflicting orders
- Supports better handoffs after inpatient stays or ED visits
- Improves adherence to transition of care protocols
- Integrated data keeps everyone aligned on the plan, which lifts both safety and experience.
Chronic disease and condition management
Chronic condition programs are doing a great job and can only continue to do so if they remain consistent with tracking. Population health analytics combined with integrated data provide you with the ability to observe tendencies not only in patients individually but also in groups. You can:
- Track clinical values and medication adherence over time
- Identify those who are losing control and offer help in time
- Compare interventions between different sites and improve protocols
When integrated data is channeled into dashboards, alerts, and workflows that clinicians both trust and use, healthcare data, driven population health becomes very effective.
Quality, performance, and value based contracts
Many organizations handle a lot of contracts. Every one of them has different rules for measurements and attribution. Through population health management, integrated data helps:
- Same calculation of measures for various payers and programs
- Finding gaps resulting in shared savings or penalties in time
- Making plans for contract negotiations and program design
By integrating population health data, the finance, clinical and operations teams are on the same page and can easily trust the data while doing assessment and planning for the next steps.
Key Benefits for Patients and Healthcare Organizations
Combined data for population health management generates value at two levels. Patients experience more coordinated and responsive care while organizations have better insight, more efficient operations, and improved outcomes.
Patient benefits
- Less repeated questions, tests and forms across different sites
- More uniform care plans that are consistent across different settings
- Before reach, out when risks or gaps show up in data
- Help that includes social needs along with clinical issue
- Enhanced communication with care teams that are on the same page
When population health analytics combined with integrated data directs outreach, patients get contact that is in line with their history and preferences. This gains the trust and progressively raises the level of engagement.
Organizational benefits
- More accurate risk identification and cohort segmentation
- Quicker response to changes in utilization and outcomes
- Quality and contract measure gains
- Analytics, care management, and operations teams working at a greater pace
Clinical, financial, and strategic leaders being well alignedHealthcare data integration for population health additionally strengthens strategic planning. Leaders can simulate scenarios, model interventions, and understand tradeoffs with the help of insights derived from fully integrated.
Challenges and Best Practices
If seamless access to integrated data for population health management was not such a challenge, organizations would already have it set up. You confront a number of practical, technical, and cultural barriers. Having a clear strategy and proven approach lowers the risk and helps you get the results faster.
Common challenges:
- Data silos and ownership: Different departments and partners own systems, have different priorities and separate budgets.N
- on, matching identifiers: Patients, providers and locations have multiple IDs, which prevents reliable matching.
- Different data standards: Different coding systems and data formats make the integration a very complicated and fragile task.
- Data quality issues: Incomplete, old or contradictory records cause distrust in analytics.
- Security and compliance issues: Privacy laws and risk management make the process of data sharing agreements very slow.
- Limited internal capacity: Your staff is already overburdened with multiple requests and handling existing systems.
Best practices for integrated data success
A practical roadmap guides you through the process of transforming fragmented data into healthcare data, driven population health management. Major areas of focus should be:
Begin with cases where the benefits are obvious to both the clinicians and the business leaders. For instance, working to close certain care gaps, improving the performance of high priority measures, or facilitating a new risk contract. When population health data integration is tied to tangible outcomes, it is easier to gain momentum and support for it.
Set up a multi, disciplinary governance committee to oversee the integrated data. This team should comprise the clinical leadership, operations, IT, analytics, and compliance. Agree on data standards, access policies, and change management right from the start. This ensures that integrated data for population health management stay not only in line with healthcare organization’s goals but also with regulatory requirements.
The establishment of a correct link between patients, providers, and locations is core. So is data cleansing and standardization. Handling of duplicates, conflicts, and gaps must be done for clinical data integration for population health in a manner that is consistent and transparent. Quality problems should be confronted upfront which ultimately lessens rework and mistrust down the road.
Integrated data become a valuable asset only when the teams utilize it in their daily work.
You can link population health analytics with integrated data directly in EHRs, care management tools, and operational systems. Provide insights through workflows, alerts, and dashboards that sync with the team’s existing operations.
Most of the time, companies don’t want to develop and support integration capabilities all by themselves. Collaborating with a partner that specializes in healthcare data integration for population health can help you lower the technical risk and shorten the time to value.
Find professionals who have extensive healthcare experience, offer proven interoperability frameworks, and have a wide range of flexible options that can fit your environment.
Conclusion
Unified data for population health management transforms fragmented information into a valuable strategic asset. It links EHR, claims, social, and operational data into a single trusted source that enables risk identification, targeted outreach, coordinated care, and continuous improvement. Patients get more consistent, quicker support. Healthcare providers acquire clearer understanding and achieve better performance in value, based programs.
To make progress, you require more than just technology. You require a partner who comprehends healthcare workflows, standards, and limitations and who sees integration as a long, term capability rather than a one, time project. Vorro is dedicated to healthcare data integration for population health with a demonstrated, interoperability, first method. Our platform assists you in consolidating clinical data, payer data, and community information, then reintegrating it into the tools your teams use daily.
If accelerating healthcare data, driven population health is one of your organization’s priorities, you can book a meeting with Vorro to discuss an integration strategy that is aligned with your objectives.
FAQs
What is Population Health Data Integration?
Population health data integration combines clinical, claims, social, and operational data into one unified and consistent structure. It facilitates risk identification, care coordination, and population analytics by providing a single source of data, rather than each data type being kept in its own silo.
How does Population Health Data Integration Help Care Teams?
Population health data integration enables care teams to comprehensively understand each patient and cohort. In one place, they have access to diagnoses, visits, medications, lab results and social needs. This leads to improved care plans, easier care transitions and more targeted outreach.
What Data is Most Essential for Clinical Data Integration for Population Health?
Clinical data integration for population health usually begins with EHR data, claims, labs, pharmacy information, and care management notes. After that, several organizations incorporate social determinants data, community resource data, and patient, generated information to gain a deeper understanding.
How does integrated data enhance population health analytics?
Population health analytics that integrate data open to use a more diverse and less contaminated input set. Therefore, this improves risk models, cohort definitions, and performance dashboards. Besides, analysts are now spending more time creating insights and recommendations that leaders and clinicians can act on rather than reconciling data.
Why choose Vorro for healthcare data integration to support population health?
Vorro specializes in healthcare interoperability and integration. Its platform enables the creation of rapid, secure connections across EHRs, payers, and other systems, and then it distributes integrated data to the locations where teams require it. Thus, it allows you to enhance healthcare data, driven population health without exhausting your internal resources. You can find more information at Vorro.















