By Akshita Kohli · February 5, 2026
Your analytics teams are very fast. Your data is not.
Clinical, financial, and operational systems communicate in different formats, use different codes, and deliver on varying schedules. You are spending more time reconciling the data than taking action.
Unified data models in healthcare analytics provide you with a common language across the enterprise. Instead of reprocessing data for each project, you agree on a shared structure once and then extend use cases across teams, facilities, and partners.
This way, the initially scattered healthcare data becomes something that you can trust, govern, and that you can effectively use for operations. It shortens the time to discovery, it makes quality improvement more effective, and it also aids value-based care decisions.
What Are Unified Data Models
A unified data model refers to a standard, reusable template that documents how your company defines, organizes, and relates its data. For the healthcare industry, it is a method of harmonizing clinical, claims, operational, and patient-generated data into a consistent set of entities, attributes, and relationships.
Rather than each analytics project devising its own schema, a healthcare unified data model provides:
- A common definition of patients, encounters, providers, locations, and payers
- Standard methods to describe diagnoses, procedures, medications, labs, and vitals
- Reference tables for coding systems such as ICD, CPT, LOINC, and RxNorm
- Well-defined relationships between clinical events, encounters, orders, and outcomes.
Of course, you will still have source-specific ingestion logic, but everything is housed in a unified, agreed-upon healthcare data architecture.
Your BI tools, data science teams, and applications then query this shared model, not a tangled mess of source schemas.
This is the root of healthcare data standardization. You decide once what an admission is, how to determine the length of stay, and how to represent risk scores. Then you apply those decisions across the entire organization.
Role of Unified Data Models in Healthcare Analytics
Unified data models in healthcare analytics play a central role in your analytics ecosystem. They act as a bridge for ingestion, transformation, governance, and consumption to work as a single unit.
They facilitate main tasks like:
- Descriptive analytics, such as a census, throughput, and service line performance
- Quality and safety metrics that include readmissions, hospital-acquired conditions, and mortality
- Population health analytics spanning care settings and payer contracts
- Revenue and cost analytics across claims, encounters, and contracts
- Predictive models depending on consistent features and longitudinal records
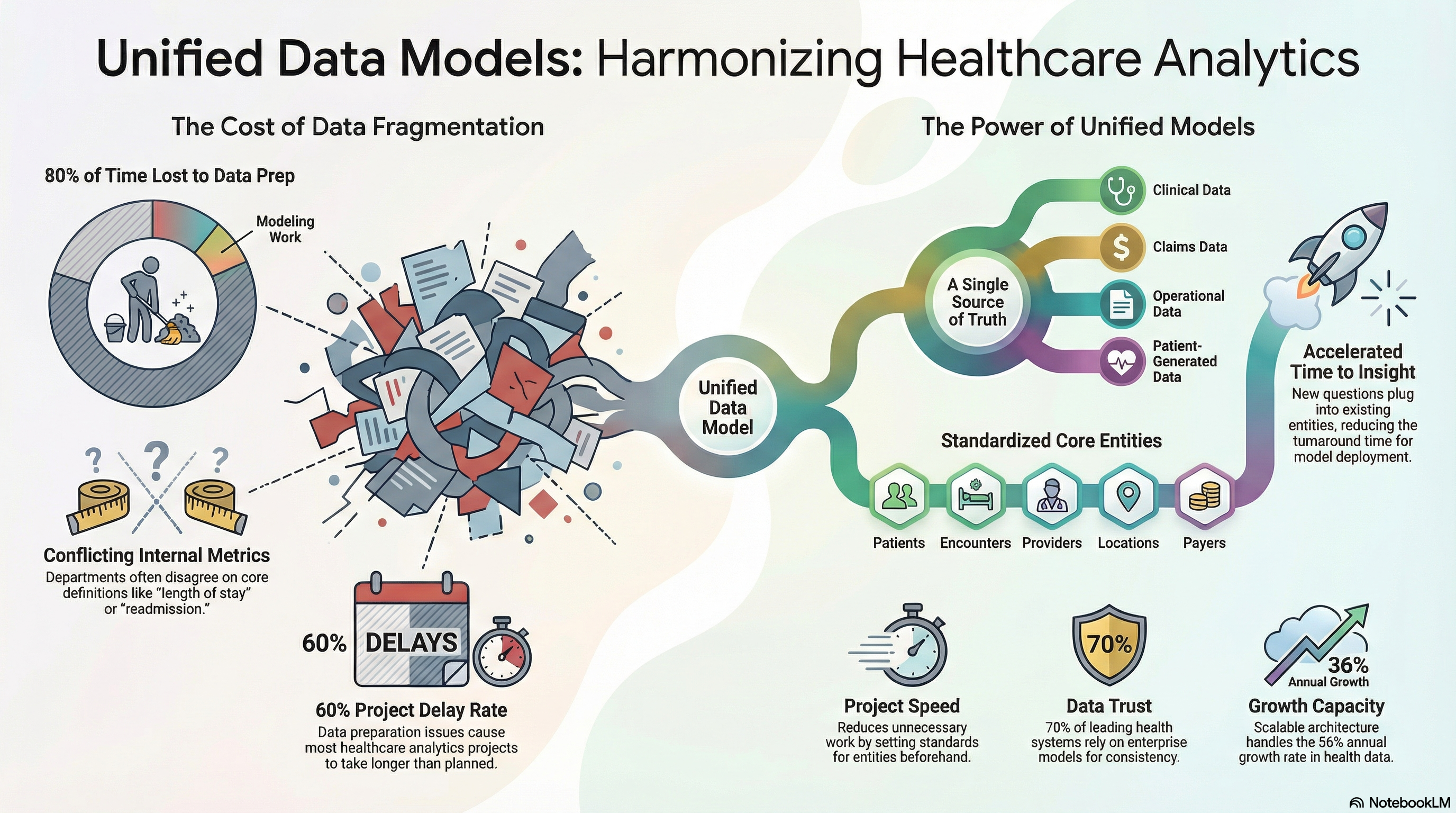
Typically, data scientists dedicate the majority of their time to preparation. According to research, analysts allocated 60 to 80 percent of their energy to data cleaning and structuring before even starting the modeling work. A single source of truth data model reduces that preparation work by setting standards for the entities and relationships beforehand.
Standardized templates are also instrumental in meeting regulatory and reporting requirements. The volume of medical records in the U.S. is increasing rapidly, and there is a prediction of a 36 percent compound annual growth rate in health data worldwide. If you don’t have a strong healthcare analytics data model, every new data source or application will inevitably put more pressure on your teams and platforms.
Challenges of Healthcare Analytics Without Unified Data Models
If analytics is done without a consolidated model, you experience the pain in several ways.
1. Fragmented definitions and metrics
Internal teams disagree on the understanding of a metric. Length of stay, readmission, or active patient metrics differ from one department, service line, or analyst to another. Reports from different teams never match, which results in a loss of trust in analytics.
Besides inconsistent healthcare data normalization, you have to deal with:
- Performing manual reconciliation of KPIs across dashboards
- Having the same discussions about definitions over and over again in meetings
- Having slow governance cycles for each new report
2. Slow project delivery and duplicated work
Every time a new project is initiated, it is essentially a fresh start. The teams tie the source data, set up the entities, and remake the transformations from scratch for each new use case. In the end, there is a heap of similar but slightly different data pipelines.
This delays the execution of the analytics and AI initiatives. According to a healthcare leader, data preparation issues are the reason why more than 60 percent of analytics projects take longer than initially planned. A single model eliminates all that unnecessary work.
3. Limited insights across systems and facilities
A healthcare data unified model is the only way to simplify cross-system analysis. Firstly, it is quite difficult to combine EHR data from multiple vendors; secondly, inpatient, outpatient, and post-acute care systems need to be aligned through a string of custom joins and mappings.
There are several types of questions that a patient journey requires, but due to the above situation, they get blocked, such as:
- Which pre-admission risk scores are indicative of post-discharge ED visits
- How ambulatory visit patterns relate to inpatient utilization
- How social determinants contribute to adherence and outcomes
4. Weak data governance and lineage
If you let every project operate its own model, you quickly lose clear lineage from the original data to the metric. You find it hard to answer straightforward questions like:
- Which fields supply a particular quality measure
- What is the source of a patient risk score
- How a financial KPI is computed across different systems
Such situations make audits, regulatory reporting, and changes to vendor contracts very slow. Besides, you raise the risk unintentionally when you modify the logic in one place but not in another.
How Unified Data Models Simplify Healthcare Analytics
Unified data models in healthcare analytics simplify your environment in four core ways: standardization, abstraction, reuse, and governance.
1. Standardization of structure and meaning
A unified healthcare data architecture offers standard tables and relationships. You do a single mapping of the sources into this structure, and then you can leverage those mappings for different reports and models.
Healthcare data standardization involves:
- Core entities: patient, encounter, provider, organization, payer, plan
- Clinical events: diagnoses, procedures, medication, labs, vitals, allergies
- Administrative data: scheduling, registration, billing, claims
- Reference data: code sets, units, value sets, and statuses
The code you use locally is in line with the standard vocabularies, e.g., the local lab codes are mapped against LOINC or medications to RxNorm. The Office of the National Coordinator revealed that standardized coding and exchange facilitate improvement in data quality and reuse across different settings, especially for care coordination and public health uses, which is the US Core Data for Interoperability initiative.
2. Abstraction from source system complexity
Source systems continue to change. Developers restructure their schemas, upgrade versions, or add new modules. A unified data model hides these changes behind a stable interface.
Your analytics logic and KPIs are based on the unified model, not on the raw sources. When a source changes, you modify the ingestion and mapping layer while leaving the downstream logic intact. This lowers the amount of regression testing that needs to be done, and you do not have to rewrite your reports or models so frequently.
3. Reusable transformations and business logic
By having a common healthcare analytics data model, you can implement standard business logic only once. This also includes logic for:
- Patient, to, provider or panel attribution
- Episode and care gaps definitions
- Risk score calculation and stratification
- Measure cohorts and denominator logic
Instead of each analytics team managing their own version of the story, you have tested and governed transformations that serve multiple use cases. This makes maintenance easy and helps keep the consistency across dashboards and AI models.
4. Stronger governance and observability
Unified models create an environment where data is organized around shared definitions and metadata.
Such a framework provides your governance teams with a definite point for:
- Linking policies and rules
- Following the lineage from source to metric
- Checking access and usage
- Tracking data quality by domain
Data quality problems can be considered the norm. Industry research indicated that about 1 in 3 business executives do not trust their data when making decisions due to quality issues.
Unified data models enable quality control at the level of specific domains, e.g., encounters or medications, thereby reducing the risk of overlooking dangerous areas.
Key Benefits for Healthcare Organizations
Healthcare analytics with a unified data model adoption delivers a wide range of benefits across clinical, operational, and financial outcomes.
1. Faster time to insight
Teams stop rebuilding the core structures for each new project. New questions simply plug into already existing entities and their relationships. This way, you reduce the turnaround time from making a data request to the delivery of a dashboard or a model deployment.
Health organizations that put money into modern data platforms, which include standardized models, report definite improvements. A survey, for instance, reveals that more than 70 percent of leading health systems rely on enterprise data models to facilitate analytics across functions rather than use separate silos of departments.
2. Higher data trust and usage
Clinicians and executives trust analytics more and more each time they find consistent numbers across different reports. Unified models ensure that there is only one source of truth for the core definitions.
More trust leads to greater usage. Analytics teams are no longer report factories but strategic partners since the whole organization recognizes analytics as dependable, repeatable, and not inconsistent or ad hoc.
3. Enhanced Population Health and Value, Based Care Performance
Population health initiatives require comprehensive and continuous patient information from different health care settings and payers. A unified healthcare analytics data model combines clinical, claims, and social data to create understandable patient journeys. This enables:
- Correct risk stratification and identification of care gaps
- Monitoring of performance across contracts and cohorts
- Care management workflows based on nearly real, time data
These features are essential for both outcomes and costs. A study published in the JAMA Health Forum found that better utilization of integrated clinical and claims data was associated with improved performance on value, based contracts and lower total cost of care.
4. Lower long-term data engineering and maintenance costs
Unified models lead to fewer one-off pipelines and custom schemas. You put more resources into shared foundations and less into duplicated project work.
Eventually, this will lower your technical debt. Your staff will be able to devote more energy to new capabilities rather than dealing with inconsistent definitions or reconciling reports from different systems.
Common Use Cases in Healthcare Analytics
When you decide on a healthcare unified data model, lots of use cases become available to you. Each one of them takes advantage of the same patient, encounter, and event structures as well as the same healthcare data normalization rules.
1. Enterprise quality and performance dashboards
You can integrate clinical quality measures, patient safety indicators, and operational KPIs across hospitals, clinics, and service lines. Since all measures are based on the same definitions of encounters, diagnoses, and procedures, the top management sees a consistent performance story.
You analyze:
- Readmissions, mortality, and complications by unit and provider
- Throughput metrics such as time to bed and length of stay
- Utilization of imaging, labs, and procedures
2. Population health and care management
Unified models enable risk stratification and care gap analytics that use both clinical and claims data. You pinpoint high-risk cohorts, candidates for outreach, and gaps related to specific contracts.
Care management teams get to look at a shared view of patient risk, utilization, and outcomes across systems. This not only helps align clinical work with payer expectations but also with community needs.
4. Predictive models and AI initiatives
Unified models make cost and revenue analytics more accurate when your healthcare analytics integration includes clinical events and financial data. You link:
- Encounters with departments, orders, and resources
- Charges and payments with episodes and service lines
- Contract terms with utilization and outcomes
Finance and operations teams, therefore, use consistent data to decide on things like service line investments, staffing models, and contract negotiations.
4. Predictive models and AI initiatives
Feature engineering is probably the step that takes the most time for predictive models. A unified healthcare analytics data model offers stable, well-defined features like prior utilization, chronic conditions, medication history, and lab trends.
Models can be used for:
- Readmission risk at discharge
- ED utilization risk for ambulatory patients
- No-show risk for scheduled visits
- Care management prioritization
Data engineers and data scientists align their work with the same base, which leads to faster development cycles and improved reproducibility.
5. Regulatory, public health, and research reporting
Regulators, agencies in the public health sector, and research partners need data in standard formats and with the use of standard coding.
A single scheme that is in line with healthcare data standardization efforts is a good way to cut down on the manual work of extracting and changing formats.
By way of example, adhering to the USCDI and standard vocabularies will allow you to share data with health information exchanges and public health systems that use the same definitions. It is also a great advantage for research teams as they can access the unified model directly, which means they dont have to go through each source system to gain access.
Conclusion
Unified data models for healthcare analytics convert disparate, messy data into a valuable strategic resource. They provide you with a unified structure, common definitions, and reusable transformations that can be scaled across the entire company.
By means of a robust and healthcare unified data model, you can uplift accelerated discoveries, enhanced governance, improved population health programs, and dependable predictive models. You equip your organization with data sources and regulations coming your way in the future instead of responding to each new requirement with another one-off project.
At Vorro, we empower health systems, payers, and health tech companies to come up with and utilize a unified healthcare data architecture that ties clinical, financial, and operational data into an integrated, analytics-ready model. If you want to lessen the integration work, fortify analytics, and direct your teams towards results rather than plumbing, have a discussion with Vorro about your unified data model strategy.
FAQs
What is a unified data model in healthcare?
Simply put, a unified data model represents a common, hospital-wide structure for the key entities such as patients, encounters, clinical events, finance, and others. This means they standardize tables, fields, and relationships in such a way that every analytics and integration effort derives definitions from the same source rather than creating new schemas.
How is a unified data model different from a data warehouse?
In essence, a data warehouse is a resource where data is stored and from which it can be retrieved via queries. On the other hand, a unified data model refers to the idea or plan of how the data is ordered. One may choose to bring into existence a healthcare unified data model in a warehouse, a lakehouse, or a cloud data platform. The model deals with the existence and interrelationship of objects, whereas the platform is concerned with the storage and overall system efficiency.
Why is healthcare data standardization essential for analytics?
Standardization is a key to ensuring that the meaning of diagnoses, procedures, labs, medications, and patient encounters stays consistent within and across systems and facilities. In its absence, KPIs and models are built on incompatible definitions, resulting in contradictory reports and bad decisions. The use of standard vocabularies coupled with a unified model enables you to have comparability over time, places, and different data sources.
How do unified data models facilitate healthcare analytics integration?
Unified models act as intermediaries between source systems and analytics tools. Integration pipelines convert EHR, claims, and ancillary data into the unified structure. BI tools, SQL users, and data science platforms then derive knowledge from that consistent model. This allows a significant reduction of custom integration work for each use case and makes it easier to upgrade when some sources change.
What issues should one take into account when preparing a healthcare analytics data model?
Concentrate on main entities like patient, encounter, provider, location, and payer. It is helpful to align with standards such as ICD, CPT, LOINC, and RxNorm. The model should be able to support a longitudinal patient view across various settings and payers. Also, think about making it extensible so it can be easily combined with devices, patient-reported outcomes, and other new data sources. Besides that, consult clinical, operational, and analytics stakeholders so the model mirrors actual workflows and decision needs in the world.














